Is it just snoring, or is something more serious going on?
You’re tired all the time. Your partner complains about the noise. You’re starting to wonder if that disruptive snoring and constant daytime fatigue are just annoyances or signs of a deeper problem. The first step toward finding out is a simple, structured self-assessment right at home. It’s all about looking past the noise to connect the dots between key symptoms and your personal risk factors.

It’s incredibly common to write off loud, chronic snoring as just an irritating habit. But in my experience, it's often the most obvious red flag that something is physically blocking your airway while you sleep. Simple snoring happens when air squeezes through a partially narrowed passage. Sleep apnea is different—it involves repeated, complete blockages.
That distinction is critical. When your airway closes, your brain senses the dangerous drop in oxygen and jolts you just enough to gasp for air. This can happen dozens, or even hundreds, of times a night, completely wrecking your sleep quality without you ever fully waking up.
Recognizing the Telltale Symptoms
Your body leaves a trail of clues that go far beyond just the sound of snoring. Many people with undiagnosed sleep apnea live with a consistent set of symptoms that, when viewed together, point directly to the condition. Think of these not as separate issues but as pieces of a larger puzzle.
Here are the key warning signs I tell people to watch for:
- Witnessed Apneas: This is a big one. Has a partner or family member ever told you that you stop breathing, gasp, or choke in your sleep?
- Morning Headaches: Waking up with a dull, throbbing headache is a classic sign of low oxygen levels overnight.
- Excessive Daytime Sleepiness: This isn’t just feeling a bit tired. It’s an overwhelming urge to doze off during the day, even after what felt like a full night in bed.
- Irritability and Mood Swings: When your sleep is constantly fragmented, your emotional regulation and mental clarity take a direct hit.
- Difficulty Concentrating: You might find yourself struggling to focus at work or forgetting simple things you normally wouldn't.
Connecting Risk Factors to Your Experience
While symptoms tell you what’s happening, risk factors help explain why it might be happening. Certain physical traits and lifestyle habits significantly increase your chances of developing obstructive sleep apnea. Identifying these is a crucial part of your initial at-home check-in.
One of the strongest physical predictors is a large neck circumference—that’s typically more than 17 inches for men and 16 inches for women. Extra tissue in the neck area can easily collapse and block the airway when you lie down. In the same way, being overweight or obese often means more fatty deposits around the throat, narrowing that crucial breathing passage.
Other important risk factors to consider are:
- Age: Risk goes up as we get older, simply because muscle tone in the throat naturally decreases.
- Family History: Unfortunately, there can be a genetic component that makes you more susceptible.
- Anatomy: Things like a narrow throat, large tonsils, or a recessed jaw can physically predispose you to airway obstruction. You can learn more about how these factors play a role in our detailed guide on what obstructive sleep apnea is.
- Alcohol or Sedative Use: These substances relax your throat muscles, making airway collapse far more likely.
- Smoking: The inflammation caused by smoking can lead to swelling in the upper airway, making a tight space even tighter.
Obstructive sleep apnea is a widespread issue, affecting a significant portion of the population. The American Academy of Sleep Medicine estimates it impacts around 54 million adults in the U.S. alone. While awareness is high, with over 76% of diagnosed individuals viewing it as a serious health risk, a concerning 40.3% have not pursued treatment. This highlights a major gap between knowing there's a problem and taking action. You can explore the full technical guidelines and prevalence data in this comprehensive AASM report.
Your At-Home Sleep Apnea Screening Toolkit

Okay, you’ve connected the dots between your symptoms and risk factors. Now it’s time to move from a hunch to gathering some real data. This is where we bring in a few clinically validated tools that help quantify what you're experiencing in a way that sleep specialists understand.
We're going to focus on two incredibly useful questionnaires and the simple but powerful practice of keeping a sleep diary. Think of this as building a case file—translating feelings of exhaustion and your partner’s complaints into measurable information. This is a critical step in figuring out if sleep apnea is what's really going on.
The STOP-Bang Questionnaire: Your First Checkpoint
The STOP-Bang questionnaire is a go-to screening tool for obstructive sleep apnea (OSA) in the medical community. It's respected because it's fast, straightforward, and surprisingly accurate at flagging people who are at high risk. The acronym itself is a handy way to remember the key questions.
Take a moment to answer the questions in the table below. Each "Yes" counts as one point.
STOP-Bang Questionnaire Self-Assessment
| Question (Acronym) | Description | Your Answer (Yes/No) |
|---|---|---|
| Snoring | Do you snore loudly (loud enough to be heard through closed doors or from another room)? | |
| Tired | Do you often feel tired, fatigued, or sleepy during the daytime? | |
| Observed | Has anyone observed you stop breathing, gasp, or choke during your sleep? | |
| Pressure | Do you have or are you being treated for high blood pressure? | |
| BMI | Is your Body Mass Index (BMI) greater than 35 kg/m²? | |
| Age | Are you over 50 years old? | |
| Neck | Is your neck circumference greater than 16 inches (40 cm)? | |
| Gender | Are you male? |
So, what's your score? A total of 3 or more suggests an increased risk for OSA. If you scored 5 or higher, there’s a high probability you're dealing with moderate to severe sleep apnea. Remember, this isn't a diagnosis, but it’s a very strong signal that it's time to talk to a professional.
Gauging Daytime Sleepiness with the Epworth Scale
While STOP-Bang zeroes in on your physical risk factors, the Epworth Sleepiness Scale (ESS) measures the real-world impact on your daily life. It asks you to rate your chances of dozing off in eight common situations, giving a hard number to just how severe your daytime sleepiness has become.
You'll rate each scenario on a simple scale: 0 (would never doze) to 3 (high chance of dozing).
- Sitting and reading
- Watching TV
- Sitting inactive in a public place (like a theater or a meeting)
- As a car passenger for an hour without a break
- Lying down to rest in the afternoon
- Sitting and talking to someone
- Sitting quietly after lunch (no alcohol)
- In a car, while stopped for a few minutes in traffic
Add up your points. A total score of 10 or higher is a clear indicator of significant sleepiness and warrants a deeper look. This score is a powerful piece of evidence to bring to a doctor, as it shows exactly how your sleep quality is affecting your waking hours.
Your screening scores work together to tell a story. For example, a high STOP-Bang score plus a high Epworth score paints a pretty clear picture: you have the classic physical risks for sleep apnea, and it's seriously compromising your ability to stay alert. That combination is often the wake-up call people need to seek real answers.
The Power of a Detailed Sleep Diary
Finally, let's talk about keeping a sleep diary. This is so much more than just jotting down when you went to bed. For the next week or two, your mission is to create a detailed log that reveals the hidden patterns of your sleep and its fallout.
Here's what you should track every day:
- Bedtime and Wake-Up Time: Be precise.
- Estimated Sleep Duration: How many hours do you think you actually slept?
- Snoring Intensity: Use a 1-10 scale. This is where a partner’s input is gold.
- Witnessed Events: Ask your partner to note any gasping, choking sounds, or noticeable pauses in your breathing.
- Daytime Fatigue Levels: Rate your sleepiness on a 1-10 scale at different times—morning, afternoon, and evening.
- Other Symptoms: Make a note of any morning headaches, a dry mouth, or a sore throat when you wake up.
This day-by-day tracking brings patterns to the surface. One rough night is just life, but a full week of loud snoring, observed apneas, and crippling daytime fatigue provides the kind of concrete data that you and your doctor can work with. It transforms vague complaints into a documented history.
Using Wearables to Uncover Nighttime Clues
Your questionnaires and sleep diary give you a solid starting point based on how you feel. But what if you could add hard data to back it up? This is where technology you might already have, like a smartwatch or fitness ring, can be incredibly revealing.
These devices give us a window into what’s happening in your body overnight, picking up on clues that are otherwise invisible. Now, let’s be clear: these are not medical diagnostic tools. It's crucial to understand their limitations right from the start.
However, they are fantastic for spotting trends and red flags. The main thing we’re looking for here is your blood oxygen saturation, which you’ll probably see displayed as SpO2.
What Your Wearable Is Really Measuring
So how does your watch know your oxygen levels? Most modern wearables use a technology called photoplethysmography (PPG). It's a fancy term for a simple process: tiny lights on the back of the device shine into your skin, and a sensor measures the light that bounces back.
Because blood with plenty of oxygen absorbs light differently than blood without, the device can estimate your SpO2 levels.
When someone has sleep apnea, their airway closes off, causing them to stop breathing for short bursts. This makes their blood oxygen levels plummet. If your watch shows repeated, significant dips in your SpO2 all night long, that’s a powerful sign that something is interfering with your breathing.
Using an Overnight Pulse Oximeter
While many smartwatches track SpO2, a dedicated overnight pulse oximeter is often the better tool for the job. These are usually small, simple devices that slip onto your finger and are designed specifically for continuous monitoring while you sleep. They tend to give more reliable data.
To get the most out of one, here’s what I tell my patients:
- Get a Snug Fit: The device should be secure but not so tight that it’s uncomfortable or cuts off circulation. A loose fit will give you messy, inaccurate readings.
- Charge It Up: Make sure it’s fully charged before bed. You need it to record for at least 8 hours straight to get a complete picture.
- Settle in First: Before you hit "record," lie still for a few minutes. This lets the device get a stable baseline reading before you drift off.
- Gather a Few Nights of Data: One night is just a snapshot. You need to look for patterns. I always recommend recording for at least 3-5 consecutive nights to see if the issue is consistent.
Each morning, sync the data to its app. You aren't just looking for one low number; you're searching for a pattern of drops and recoveries. Seeing your oxygen levels repeatedly fall from a healthy 96% down into the 80s is a major red flag and something you absolutely need to discuss with a professional.
How to Interpret the Data (Cautiously)
Remember, the data from your wearable is supporting evidence, not a final diagnosis. A "sleep score" in an app is just a branded algorithm, not a true medical metric. Your focus should be on the raw numbers that can point to breathing disruptions.
Key Takeaway: The goal here isn't to diagnose yourself at home. It's to gather objective data that confirms your symptoms. A consistent pattern of oxygen drops is a very compelling reason to seek a professional evaluation.
This kind of at-home screening is becoming the standard way people first discover a problem. In fact, a 2023 survey found that a staggering 66.7% of U.S. adults with sleep apnea initially identified their condition using at-home testing methods. This just goes to show how accessible tech is empowering people to take that first step. You can read more about it in the full SleepApnea.org report.
When you pull all this information together, organize it. Take screenshots of the graphs showing your SpO2 levels. Note the dates and any important context—for instance, if you had a drink before bed, which is known to make apnea worse.
When you combine these objective numbers with your questionnaire scores and sleep diary, you build a powerful, multi-faceted case. This is exactly the kind of organized evidence a sleep specialist needs to see to decide on the right next steps for a formal diagnosis.
Putting the Pieces Together (Without Self-Diagnosing)
Okay, so you've tracked your symptoms, worked through the questionnaires, and gathered a bunch of data from your sleep tracker. You're holding a pile of clues. The goal now isn't to diagnose yourself, but to organize these clues into a clear story for a medical professional. You're building an evidence-based case for getting a proper evaluation.
Let's walk through a common scenario we see all the time. Your partner complains about your loud, disruptive snoring—that’s clue number one. You then take the STOP-Bang questionnaire and score a 5, and your Epworth Sleepiness Scale comes back at a 12. These scores flag you as high-risk and confirm that, yes, your daytime fatigue is a real problem.
To top it off, you look at your wearable data and see your SpO2 levels dipping into the high 80s, night after night.
When you connect those dots, the picture becomes hard to ignore. Your subjective experiences (snoring, feeling exhausted) are now backed up by validated screening tools and objective data (oxygen drops). This isn't just a hunch anymore; it's a documented pattern that screams for a professional opinion.
Avoiding Common Pitfalls in Interpretation
As you piece things together, it’s really important to keep your perspective. It's easy to see some scary numbers and jump to conclusions, but your at-home screening has its limits.
One of the biggest mistakes is fixating on a single bad night. Did you have a few beers before bed? Are you coming down with a cold? Both can temporarily mess with your breathing and oxygen levels. That’s exactly why we recommend collecting data for at least a week—it helps you separate a fluke from a genuine, consistent problem.
Another trap is getting too hung up on a "sleep score" from your favorite app. These scores can be great for motivation, but they're based on proprietary algorithms. They don't measure the clinical markers that truly define sleep apnea, like airflow or respiratory effort.
Instead, focus on the raw data that actually matters:
- How often are you having loud snoring events?
- Do you see a pattern of SpO2 drops (desaturations)?
- Are your fatigue scores in your sleep diary consistently high?
Think of yourself as an investigator building a case file, not the judge delivering a verdict. Your goal is to gather enough solid evidence to justify a formal medical test. The final diagnosis has to come from a qualified professional.
This chart helps visualize how your clues—snoring and oxygen data—point you toward the next step: seeing a doctor.
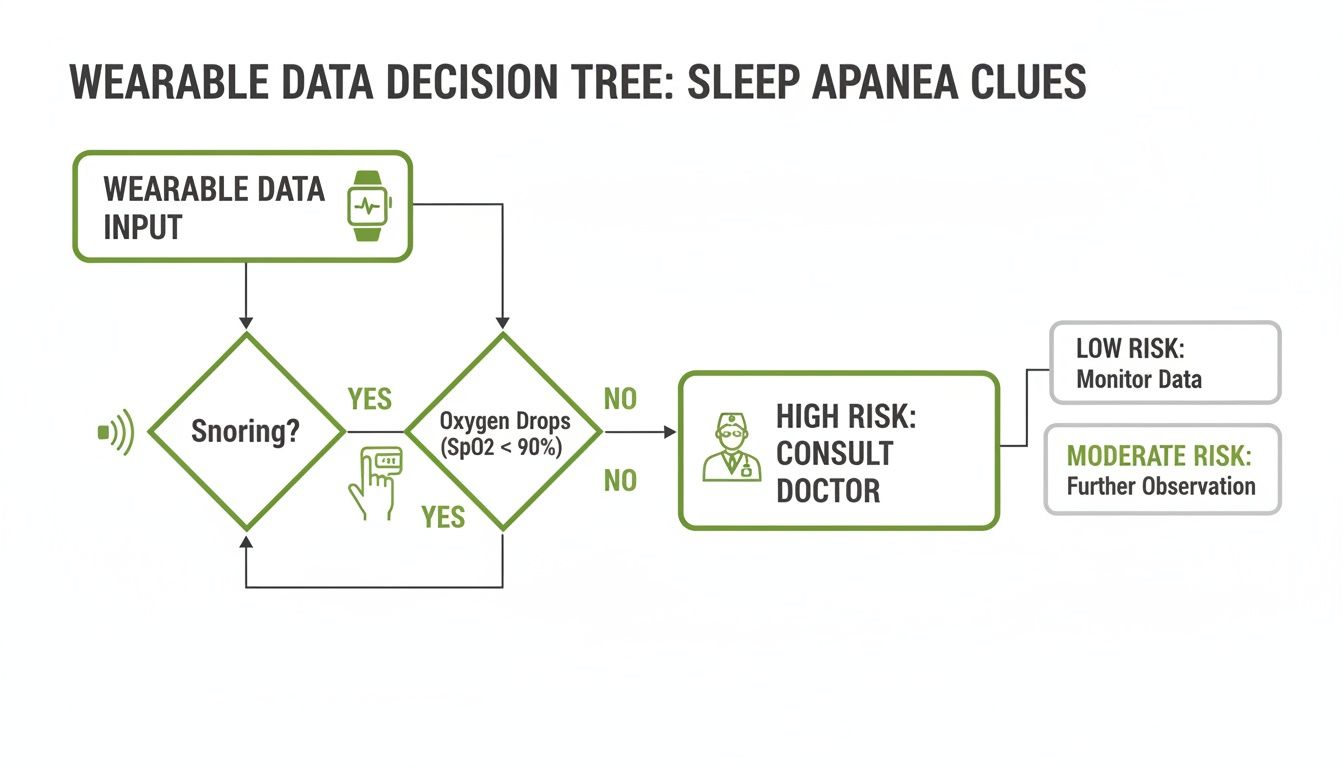
It really just reinforces the main takeaway: if you're consistently snoring and seeing oxygen drops on your wearable, it’s time to get a professional involved.
Your Screening vs. a Formal Home Sleep Apnea Test
It's crucial to understand the difference between what you've been doing and a formal Home Sleep Apnea Test (HSAT). Your at-home work is a preliminary risk assessment. An HSAT is a medical diagnostic tool, prescribed by a doctor like Dr. Larson here at the Pain and Sleep Therapy Center.
While your watch or ring gives you a glimpse into your oxygen levels, a medical-grade HSAT measures much more, including:
- Nasal Airflow: To actually detect when you stop breathing.
- Respiratory Effort: To see if your body is still trying to breathe during an apnea event.
- Blood Oxygen Saturation: Measured with a medical-grade sensor for accuracy.
- Heart Rate: To track how your cardiovascular system responds to these events.
This is the detailed, clinical-level data a specialist needs to officially diagnose sleep apnea and figure out how severe it is. These medical tests have over 90% accuracy for spotting moderate to severe cases. While they capture about 85% of what an in-lab study does, they can sometimes underestimate the severity because of how they measure time. You can read more about the reliability of at-home sleep tests on sleepandsinuscenters.com.
Ultimately, all the diligent work you’ve done at home provides the compelling evidence your doctor needs to order one of these definitive tests.
Knowing When to See a Sleep Specialist

You’ve gathered the clues and organized your notes. Now comes the most important part: turning your self-investigation into a real conversation with a medical professional. The whole point of this at-home detective work is to know exactly when to stop guessing and get an expert opinion.
If your screening has raised some red flags, that’s your signal. This isn't about jumping to conclusions; it’s about being proactive with your health. Ignoring the signs can lead to serious long-term consequences, but taking the next step can put you on a path to feeling better than you have in years.
Time to Make the Call
Deciding to book a consultation can feel like a big move, but it's the logical next step if your data is pointing in that direction. Your personal screening has given you a solid foundation—now it’s time to hand that intel over to an expert who can give you a definitive diagnosis and a clear plan.
It’s time to schedule that appointment if you’re seeing any of these patterns:
- High Questionnaire Scores: A score of 3 or more on the STOP-Bang or 10 or more on the Epworth Sleepiness Scale is a strong sign you need professional input.
- Concerning Wearable Data: You’ve recorded multiple nights where your blood oxygen (SpO2) dips below 90%, especially if you see a pattern of repeated drops and recoveries.
- Serious Daytime Impairment: Your fatigue is more than just feeling tired. It’s affecting your work, your relationships, or your ability to drive safely.
- Partner Observations: This is a big one. If your partner consistently says you stop breathing, gasp, or choke in your sleep, it's one of the most compelling reasons to get checked out.
If any of this sounds familiar, your at-home work has done its job. You have the evidence you need to seek a formal evaluation.
What to Expect From a Professional Consultation
Making that call to a specialty clinic like the Pain and Sleep Therapy Center might feel intimidating, but we design the process to be straightforward and supportive. You aren't starting from scratch. You're walking in with a well-documented case file that gives a specialist, like Dr. Larson, a huge head start.
During your first consultation, we'll talk through your symptoms, review your screening results, and go over your health history. It’s this conversation that helps us map out the best diagnostic path for your specific situation.
The goal isn't just to get a diagnosis; it's to understand the why behind your sleep issues. A true evaluation looks at the whole picture—your anatomy, breathing patterns, and lifestyle—to build a treatment plan that addresses the root cause, not just the symptoms.
Based on this comprehensive review, the specialist will recommend the most appropriate next step, which can vary depending on your unique case.
The Path to a Formal Diagnosis
Once you're working with a sleep specialist, they will use your information to order a medical-grade test. For many people showing classic signs of obstructive sleep apnea, that means a Home Sleep Apnea Test (HSAT). This is a more advanced, FDA-approved device you use in your own bed to get a precise, clinical diagnosis.
In other cases, especially if there are other health conditions like heart or lung disease, an in-lab sleep study, or polysomnography, might be the right call. This is the gold standard for diagnosis, as it monitors many more signals, including brain wave activity.
The key takeaway is that you don’t have to figure this out alone. The results from a formal test will give your doctor the data needed to recommend effective treatment. Fortunately, for those who struggle with traditional methods, it’s worth exploring how sleep apnea treatment without CPAP can offer real relief through custom oral appliances and other therapies. Your journey to better sleep starts with this single, decisive step.
Your Top Questions About At-Home Sleep Apnea Screening, Answered
Once you start digging into the world of at-home sleep apnea screening, a lot of questions pop up. It's totally normal to wonder what the data you're collecting actually means, how accurate it is, and what to do with it. Let's clear up some of the most common questions we hear from patients.
How Accurate Are Smartphone Apps and Wearables?
Think of these consumer gadgets as fantastic early-warning systems, not medical diagnostic tools. They're great for spotting trends—like frequent snoring or dips in your blood oxygen levels overnight—but they just don't have the sophisticated, medical-grade sensors needed to measure things like airflow and breathing effort. Without that, you can't get a formal diagnosis.
The data they provide is incredibly useful for building a case to bring to your doctor. If your watch consistently shows oxygen drops, that’s a compelling reason to seek a professional opinion. Just remember, the app itself can't officially diagnose sleep apnea.
What’s the Difference Between Home Screening and a Formal HSAT?
This is a crucial distinction. The "home screening" we've been walking through in this guide is what you do on your own. It’s your personal investigation using questionnaires, sleep diaries, and consumer tech to figure out your risk level.
A formal Home Sleep Apnea Test (HSAT), on the other hand, is a medical test prescribed by a doctor. It involves a specific, FDA-approved device that measures key biological signals—airflow, breathing effort, blood oxygen, and heart rate—to gather the clinical data needed for a real diagnosis.
Key Takeaway: Your personal screening builds the evidence you need to show your doctor why a formal HSAT is a good idea. One is an informal investigation; the other is a prescribed medical test.
So, I Can’t Just Diagnose Myself at Home?
That’s right, and for good reason. A formal medical diagnosis has to come from a qualified healthcare professional. While the steps in this guide give you a powerful look at your personal risk, only a doctor can interpret the data from an HSAT in the context of your complete health profile.
This is a critical safety step. An expert evaluation makes sure other potential health problems aren't missed and ensures you get a treatment plan designed specifically for you, not just a one-size-fits-all solution.
My Screening Results Are Concerning. What's Next?
If your self-assessment is pointing toward a high risk of sleep apnea, it's time to turn your data into action. Your next move is to book a consultation with a sleep specialist.
Gather up everything you've collected and bring it to your appointment. This is your evidence file!
- Your scores from the STOP-Bang and Epworth Sleepiness Scale.
- Your sleep diary, with at least one or two weeks of detailed notes.
- Screenshots or printouts from your wearable, highlighting any nights with blood oxygen drops or other unusual patterns.
Handing this over to your doctor gives them a massive head start. It helps them see the full picture right away and map out the quickest path to a formal diagnosis—and ultimately, to getting you the good sleep you deserve. As you move forward, you might also want to look into the best exercises for sleep apnea to help support your treatment and improve airway health.
At the Pain and Sleep Therapy Center, we specialize in providing clear answers and personalized treatment plans that address the root cause of your sleep issues. If your home screening has raised concerns, schedule a consultation with our expert team to take the definitive next step toward reclaiming your health. Learn more at https://pscharlotte.com.





