When you're dealing with chronic pain, it's easy to get trapped in a frustrating cycle: find a fix for one symptom, only to have the pain pop up again somewhere else. This isn't just you—it's a common pitfall in traditional pain care, where the focus is often on quieting the loudest symptom instead of finding the root cause.
Why Traditional Pain Treatments Often Fail
This narrow approach often leads to a hamster wheel of temporary relief followed by recurring pain, leaving patients feeling stuck and completely hopeless.

Think about it like this: your car’s engine light comes on. You take it to a mechanic who just checks the oil, tops it off, and sends you on your way. The light might go off for a little while, but if the real problem is a worn-out part or a bad sensor, you know that light is coming right back on.
This is exactly what happens when complex conditions like TMJ disorders or orofacial pain are treated with isolated, single-specialist methods. It’s not a failure of any one doctor, but a major limitation of a system that often treats symptoms in a vacuum.
The Disconnected Patient Journey
For someone with chronic jaw pain and morning headaches, the typical journey is all too familiar. It usually looks something like this:
- Visit 1: The Primary Care Physician. They might start with muscle relaxants or pain relievers. This can bring some comfort, but it does nothing to address what’s causing the muscle tension in the first place.
- Visit 2: The Dentist. Next up, they might make a standard night guard to protect the teeth from grinding. It’s a helpful step, but it doesn't answer the crucial question: why is the grinding happening?
- Visit 3: The Neurologist. After ruling out more serious conditions, they may offer yet another prescription to manage the headaches.
Each specialist sees a different piece of the puzzle. The primary doctor sees pain, the dentist sees worn-down teeth, and the neurologist sees headaches. They’re all correct in their own silo, but no one is stepping back to look at the whole picture. This disjointed process completely misses how jaw function, posture, breathing mechanics, and sleep quality are all connected.
Chronic pain is a massive global issue, affecting about 20% of adults worldwide. In the U.S. alone, 51.6 million adults reported living with chronic pain in 2021. This is where a multidisciplinary approach to pain management becomes a game-changer.
The evidence is clear: integrated pain clinics deliver far better results. One study showed that team-based care not only reduced prescription costs by $6.68 per patient per day but also led to fewer primary care visits and hospital stays. You can dive deeper into the research by exploring the full study on the effects of integrated pain care.
This really drives home the need for a new model of care. Instead of bouncing between appointments and trying to piece together conflicting advice, patients need a collaborative team that actually communicates and works together. This integrated strategy is the heart of a true multidisciplinary approach to pain management—one that moves beyond temporary fixes to deliver solutions that last.
What Is a Multidisciplinary Approach to Pain Management
Let’s break down what a multidisciplinary approach to pain management really means. Think of it like this: your body is a high-performance vehicle with a complex, nagging issue. Instead of taking it to a tire specialist, then an engine mechanic, and then an electrician—all working separately—you bring it to a dedicated performance center.
There, a whole team of experts inspects the vehicle together, shares diagnostic data in real-time, and builds one unified repair plan. That’s exactly how a multidisciplinary clinic works. It’s a collaborative model that brings different healthcare specialists together under one roof, all focused on your unique case.
Unlike the traditional route of seeing specialists one by one, this integrated model is built on constant communication and shared goals. It moves beyond just chasing symptoms to actually uncover and address the root causes of your pain—whether that’s a muscle imbalance, a restricted airway, or something else entirely.
A Symphony of Coordinated Care
A great way to visualize this approach is to picture a symphony orchestra. Each provider is a highly skilled musician with a specific instrument—a neurologist, a physical therapist, a dental sleep medicine expert. While each is a master of their craft, their individual efforts might sound chaotic without a leader.
In this model, a lead clinician acts as the conductor, making sure every specialist plays in harmony. This conductor coordinates the entire treatment plan, ensuring each therapy complements the others. The result is a beautiful, cohesive piece of music—or in your case, a successful and lasting health outcome.
A multidisciplinary approach recognizes that chronic pain is rarely a single-issue problem. It is often a complex web of interconnected factors, including biomechanics, neurology, and even breathing patterns. The goal is to untangle this web, not just snip at the loose threads.
This coordinated strategy ensures nothing falls through the cracks. It helps avoid the all-too-common scenario where one provider’s advice accidentally contradicts another’s, leaving you confused and stuck in the middle.
Beyond Symptoms to Root Causes
The core philosophy of a multidisciplinary team is to look deeper. For instance, chronic headaches or jaw pain might not just be a localized muscle issue. They could be the direct result of an underlying sleep-related breathing disorder that forces the jaw into a stressful position all night. To truly grasp the value of an integrated approach, it helps to first consider the complexity of common chronic issues, such as those covered in this guide to understanding back and leg pain.
A single specialist working alone might miss this critical connection. A collaborative team, on the other hand, is trained to see the bigger picture.
- The Single-Specialist View: Sees jaw pain and prescribes a mouthguard to protect the teeth.
- The Multidisciplinary View: Investigates why the jaw is clenching and discovers an airway issue. The team then works to improve breathing, which in turn reduces the strain on the jaw.
This focus on root causes is the key to achieving genuine, long-term wellness instead of just temporarily masking the pain. It’s the difference between patching a pothole and repaving the entire road for a smoother journey ahead.
Single-Specialist vs. Multidisciplinary Pain Management
The table below really highlights the fundamental differences between these two models of care. You can see how one keeps you at the center of a coordinated team, while the other often leaves you to manage the pieces yourself.
| Aspect | Single-Specialist Approach | Multidisciplinary Approach |
|---|---|---|
| Communication | Minimal to none between providers; the patient acts as the messenger. | Constant, active collaboration and shared patient records. |
| Treatment Plan | Fragmented, with each specialist creating their own separate plan. | One unified, cohesive treatment plan developed by the entire team. |
| Focus | Often targets the most obvious symptom in isolation. | Identifies and treats the underlying root causes of the pain. |
| Patient Role | Responsible for coordinating appointments and relaying information. | A central, active member of a guided and supportive care team. |
Ultimately, the multidisciplinary model is built to treat the whole person, not just a collection of symptoms. This comprehensive viewpoint is what makes it so effective for complex conditions like TMJ disorders and chronic facial pain.
Assembling Your Integrated Pain and Sleep Team
A successful approach to managing complex pain hinges on one thing: the right team. This isn't just about collecting a list of specialists; it's about building a truly collaborative force where each expert’s knowledge overlaps and strengthens the others. Think of it like a championship sports team—you need players with distinct skills who know how to work together seamlessly to get the win.
When you're dealing with something as complex as facial pain or a sleep disorder, your care team is your biggest asset. Each professional brings a unique perspective, making sure every angle of your condition is seen and addressed. This integrated strategy cuts through the conflicting advice and disjointed care that can happen in traditional treatment, putting you at the heart of a unified, powerful plan.
This diagram shows how key specialists like dentists, therapists, and neurologists can form a connected care network around you.
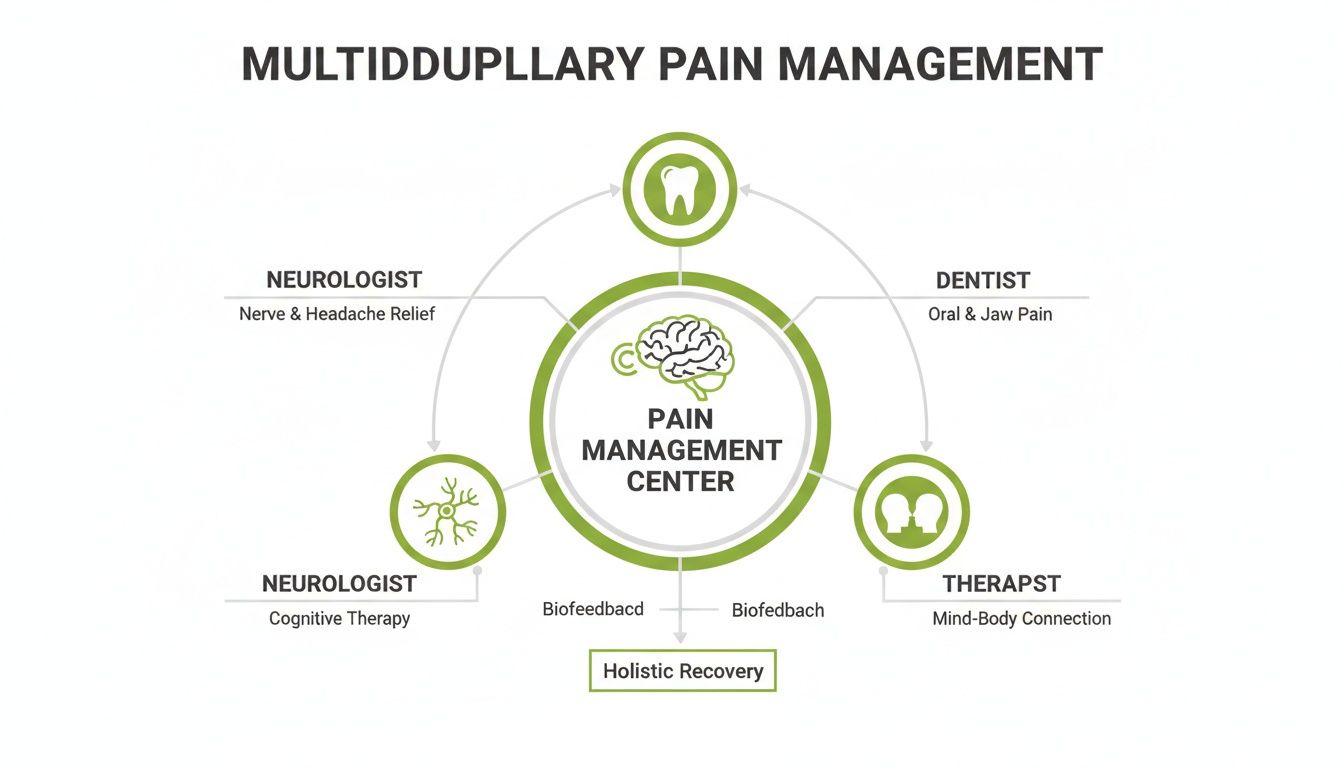
Instead of isolated appointments, this model creates a web of support where communication flows freely between your providers, all focused on a shared goal.
The Airway Architect: Dental Sleep Medicine Specialist
At the very core of many TMJ, facial pain, and sleep issues is the structure and function of your airway. The Dental Sleep Medicine specialist is the team's 'Airway Architect.' This expert has deep knowledge of oral anatomy, jaw function, and how it all directly impacts your ability to breathe, especially while you sleep.
Their main job is to evaluate and manage the physical structures that can lead to conditions like obstructive sleep apnea and TMJ dysfunction.
- Diagnostic Leadership: They often kick off the assessment, using advanced tools like 3D imaging to get a crystal-clear picture of your jaw, joints, and airway.
- Customized Oral Appliances: If a sleep-related breathing disorder is found, they design and fit custom oral appliances. These devices gently move the jaw forward to keep the airway open, offering a highly effective, non-invasive alternative to CPAP for many patients.
- Coordinating Care: The Airway Architect works hand-in-glove with the other team members, laying the anatomical foundation that other therapies build upon.
By making sure your airway is clear and functional, this specialist sets the stage for real, lasting pain relief and restorative sleep.
The Muscle and Function Coach: Orofacial Myofunctional Therapist
While the architect designs the structure, the Orofacial Myofunctional Therapist (OMT) is the 'Muscle and Function Coach.' This therapist zooms in on the intricate muscles of the face, mouth, and throat, retraining them to work correctly. So many chronic pain and sleep problems come from improper muscle habits, like an incorrect swallow, poor tongue posture, or breathing through the mouth.
An OMT is essentially doing physical therapy for your face and airway. Their work is absolutely critical for correcting the deep-seated habits that keep the cycle of pain and dysfunction going.
The OMT's job is to bring back balance and proper function through a series of targeted exercises. They focus on key areas like:
- Tongue Posture: Training the tongue to rest on the roof of the mouth where it belongs, which helps support the airway and stabilize the jaw.
- Nasal Breathing: Helping patients shift from habitual mouth breathing to much healthier and more efficient nasal breathing.
- Correct Swallowing: Retraining the swallowing pattern to take the strain off the facial and jaw muscles.
This muscle re-education is vital. It helps ensure that the benefits you get from other treatments, like an oral appliance, actually stick for the long haul. If you're looking into your options, seeing what a facial pain specialist near me can do is a great place to start.
The Nerve System Detective: Neurologist
When pain involves the complex web of nerves in the head and face, the Neurologist comes in as the 'Nerve System Detective.' Their expertise is essential for diagnosing and managing conditions where the nervous system is the main driver, such as trigeminal neuralgia, migraines, or other neuropathic facial pains.
Their role is to figure out if the pain is coming from musculoskeletal issues (like the TMJ) or from nerve dysfunction. That distinction is critical for creating a treatment plan that actually works. A neurologist can rule out more serious neurological conditions and provide targeted medical management when nerve-related pain is part of the picture.
Globally, pain research is exploding, with one model forecasting 1,031 new articles by 2027. This growing body of evidence consistently backs the multimodal strategies a multidisciplinary team provides for intertwined issues like TMJ disorders and sleep-disordered breathing, leading to better pain control and movement.
The Breathing Pattern Specialist: Buteyko Instructor
Finally, the Buteyko Breathing instructor is the team's 'Breathing Pattern Specialist.' This expert focuses on the physiology of breathing itself. They address dysfunctional patterns like chronic over-breathing (hyperventilation) or shallow breathing—habits that can throw off oxygen levels, nervous system regulation, and muscle tension all over the body.
The Buteyko method teaches simple techniques to restore calm, efficient, and natural breathing patterns. By normalizing your breathing volume and promoting nasal breathing, this specialist helps lower anxiety, improve sleep quality, and reduce the overall physiological stress that feeds chronic pain. Their work is the perfect complement to the OMT and the Dental Sleep Medicine specialist, creating a powerful synergy that addresses your health from every angle.
Evidence-Based Therapies That Heal and Restore
Once your expert team is assembled, the focus shifts from the "who" to the "what"—the specific, evidence-based treatments they'll use to get you better. A modern multidisciplinary approach to pain management relies on a powerful toolkit designed to accurately diagnose, heal damaged tissues, and restore proper function for the long haul. This isn't about slapping on a temporary fix; it's about creating lasting change from the inside out.
The journey starts with a deep, comprehensive look at your unique anatomy and physiology. This foundational step ensures every decision is based on solid data, not just an educated guess.

Think of this initial diagnostic phase like creating a detailed blueprint before starting construction. It reveals the hidden connections between your pain, sleep, and breathing that will guide the entire treatment strategy.
Advanced Diagnostics: The Starting Point
To truly understand the root cause of your symptoms, the team needs to see what’s happening beneath the surface. Vague symptoms like jaw pain or headaches can come from a dozen different places, so precision is everything.
This is where advanced diagnostic tools come into play, giving us an incredibly detailed picture of your health.
- 3D Cone-Beam Computed Tomography (CBCT): This imaging technology is light-years beyond a standard dental X-ray. It creates a complete three-dimensional model of your skull, jaw, joints, and airway, allowing specialists to measure airway volume and spot subtle structural issues that other scans would completely miss.
- Home Sleep Studies: These convenient, take-home tests monitor your breathing, oxygen levels, and sleep patterns right in your own bed. The data gathered is critical for diagnosing sleep-related breathing disorders like obstructive sleep apnea—often a major driver of facial pain.
These tools give your team the objective data they need to build a diagnosis that is both accurate and complete.
Regenerative Therapies: Rebuilding and Repairing
With a clear diagnosis in hand, the next step is often to address tissue damage and inflammation directly. This is where regenerative therapies shine, using your body's own natural healing abilities to repair joints and ligaments without invasive surgery.
Think of these treatments as giving your body the raw materials and the spark it needs to rebuild itself. Instead of just masking pain with medication, these therapies promote true healing right at the cellular level.
These innovative approaches represent a huge shift in pain care. The goal isn't just to manage symptoms but to fundamentally improve the health and integrity of the affected joint tissues, fostering real strength and resilience.
Two of the most effective regenerative therapies we use in a multidisciplinary setting are:
- Prolotherapy: This involves injecting a natural solution (often containing dextrose) into weakened ligaments and tendons around a joint. This creates a mild, controlled inflammatory response that signals the body to send growth factors to the area, kick-starting the repair process and strengthening the joint.
- Platelet-Rich Fibrin (PRF): PRF therapy uses a concentration of platelets and growth factors drawn from your own blood. When this "liquid gold" is injected into an inflamed or damaged area like the TMJ, it delivers a powerful dose of healing components that reduce inflammation and support tissue regeneration.
To learn more about how these treatments can help, check out our detailed guide on regenerative medicine for joint pain. This synergy is what makes a multidisciplinary approach to pain management so effective—regenerative therapies calm the joint, which then allows functional therapies to work much better.
Functional Therapies: Restoring Correct Movement
Healing the joint tissue is only half the battle. If the underlying muscle habits and breathing patterns that caused the problem in the first place aren't corrected, the pain is just going to come back. This is where functional therapies come in, acting as a specialized physical therapy for your face, tongue, and airway.
These therapies retrain your body to function the way it was designed to, breaking the cycle of strain and dysfunction for good. They are active, exercise-based treatments that empower you to take control of your own recovery.
Key functional therapies include:
- Orofacial Myofunctional Therapy (OMT): This therapy focuses on correcting improper muscle function and habits. An OMT works with you on exercises to achieve proper tongue posture, correct swallowing patterns, and establish healthy nasal breathing.
- Buteyko Breathing: Many people with chronic pain unknowingly have dysfunctional breathing patterns, like habitual over-breathing. The Buteyko method retrains you to breathe more efficiently, which helps calm the nervous system, improve oxygen delivery, and reduce overall muscle tension.
By combining regenerative and functional therapies, your team addresses both the structural damage and the dysfunctional habits, paving the way for complete and lasting relief. As you explore ways to heal and restore, you can also look into the benefits of sauna for pain relief as a great complementary method for managing inflammation and muscle soreness.
Your Patient Journey in an Integrated Clinic
Understanding how a multidisciplinary approach to pain management works in theory is one thing, but seeing it in action is what really matters. Stepping into an integrated clinic turns what can be a confusing, frustrating process into a clear and supportive journey.
Think of it less like bouncing between disconnected appointments and more like a guided expedition. You have a team of experts, all working together, dedicated to helping you reach your destination: better health. Your experience is carefully mapped out, with each phase building on the last to ensure nothing gets missed.
Phase 1: The Comprehensive Assessment
Your journey starts with a thorough investigation. This isn't just a quick look at your main symptom; it's a deep dive into your health history, lifestyle, and personal goals, combining your story with advanced diagnostics.
This is a data-gathering phase. We’ll use tools like 3D imaging to map your airway and jaw structure, and we’ll have a detailed conversation about your sleep quality. To get a clearer picture of what’s happening at night, your team might suggest you learn how to diagnose sleep apnea at home, which can offer valuable clues. The goal here is to create a complete, 360-degree view of your health.
Phase 2: The Collaborative Diagnosis
Once all the information is on the table, your expert team comes together. This is where the collaborative magic of the multidisciplinary model happens. Specialists from different fields—like dental sleep medicine, orofacial myofunctional therapy, and neurology—review your case as a group.
They share insights and connect the dots between symptoms that might seem unrelated. This process leads to a single, unified diagnosis, preventing the fragmented and often conflicting opinions you get from seeing specialists one by one. It ensures everyone is on the same page, working from the same blueprint.
This collaborative phase is where the breakthroughs occur. A jaw specialist might spot an anatomical issue, while a myofunctional therapist identifies a harmful muscle pattern contributing to it. Together, they see the whole picture.
Phase 3: The Personalized Treatment Plan
With a clear diagnosis, the team creates a personalized treatment plan just for you. This isn’t a one-size-fits-all protocol. It’s a strategic, sequenced plan that outlines which therapies to start with and how they’ll build on each other for the best results.
For example, your plan might begin with regenerative injections to calm joint inflammation. This could be followed by a custom oral appliance to support your airway, and then functional therapy to retrain muscle habits once the pain has subsided. You’ll walk away with a clear, step-by-step plan you understand and feel confident about.
Phase 4: Coordinated Care and Progress Monitoring
Your treatment begins, but the collaboration doesn't stop there. The team stays in constant communication, monitoring your progress and making adjustments as needed. If one therapy isn’t yielding the expected results, the team can quickly pivot and adapt the plan.
This active management ensures you’re always on the most effective path forward, with a dedicated team guiding you every step of the way toward lasting relief.
A Few Common Questions About Integrated Pain Care
It's one thing to understand the idea of a multidisciplinary approach to pain management, but it's another to know how it works in the real world. You probably have a few questions about the process, the logistics, and what truly makes this kind of care different.
Let's walk through some of the most common questions we hear. Our goal is to clear up any confusion and give you a better feel for how effective this model is for complex issues like TMJ disorders and facial pain.
How Is This Different From Just Seeing Multiple Specialists?
This is the most important question we get, and the answer comes down to one word: collaboration.
When you see different specialists on your own, you become the project manager. You’re the one carrying records from office to office, trying to connect the dots and explain what one doctor said to another. It’s often a frustrating process that can lead to conflicting advice and fragmented care.
In a multidisciplinary clinic, your entire team is under one roof, communicating constantly. They review your case together, share insights, and build a single, unified treatment plan from day one. It’s the difference between hiring a plumber, an electrician, and a carpenter separately versus having a general contractor who makes sure the whole house is built correctly. This coordinated approach creates a much smoother and more effective path to getting better.
Will My Insurance Cover These Integrated Treatments?
Insurance coverage can be tricky and really depends on your specific plan. Many parts of a multidisciplinary plan, like specialist consultations or diagnostic imaging, are often covered. Other therapies, especially more advanced or functional treatments, might have different rules.
The best first step is always a direct conversation with the clinic. A good multidisciplinary center will have a dedicated financial coordinator ready to help you sort through your benefits.
This person is your advocate. They'll handle the pre-authorizations, clearly explain any out-of-pocket costs, and walk you through payment options to make sure care fits your budget. Their job is to manage the financial side so you can focus completely on your health.
What If I Only Have TMJ Pain but No Sleep Issues?
This is a great question because it gets to the heart of how interconnected our bodies are. The jaw, airway, tongue, and neck are all linked. It’s very common for an underlying issue, like a restricted airway or poor tongue posture, to be the real driver of TMJ pain—even if you don't have obvious sleep symptoms like snoring.
Think of it as a quiet chain reaction. A narrow airway might cause your jaw to shift forward slightly all night long just to help you breathe better. Over time, that constant, low-level strain puts a ton of pressure on your jaw joints, leading to inflammation and pain. A multidisciplinary assessment is designed to uncover exactly these kinds of hidden root causes. By improving your airway function and muscle balance, we can often take the chronic strain off your jaw and provide a deeper, more lasting relief than treatments that only focus on the joint itself.
How Do I Know If I Am a Good Candidate for This Approach?
You are likely an excellent candidate for a multidisciplinary approach to pain management if any of these sound familiar:
- You’ve been dealing with chronic facial pain, jaw pain, or headaches, and nothing you’ve tried with a single specialist has worked.
- You’ve been diagnosed with sleep apnea and are looking for effective alternatives to CPAP.
- You have a gut feeling that your symptoms are all connected and that previous doctors might have missed the bigger picture.
The best way to know for sure is to schedule an initial consultation. That first comprehensive evaluation is designed to figure out if our integrated model is the right solution to help you finally get back to feeling like yourself.
At the Pain and Sleep Therapy Center, our entire team is focused on finding the root cause of your pain and sleep problems. We’re committed to providing a truly integrated care experience that leads to lasting relief. If you're ready to move beyond quick fixes, we invite you to schedule a consultation and start your journey toward better health.





