Think of a TMJ flare-up as your jaw’s way of saying it’s had enough. That sudden, intense pain is your body's signal that the jaw joint and its surrounding muscles are overloaded. More often than not, the culprit isn’t a single event but a perfect storm of accumulated stress.
The most common causes are stress-induced clenching during the day, unconscious nighttime teeth grinding (bruxism), and even simple daily habits like chewing tough foods or maintaining poor posture. Over time, these factors build on each other, leading to muscle fatigue, inflammation, and that all-too-familiar jaw pain.
Decoding the Triggers Behind Your Jaw Pain
Your jaw joint is a remarkably complex intersection where muscles, nerves, and bone work together. When everything is functioning correctly, it’s seamless. But certain triggers can create a massive "traffic jam," leading to the gridlock we call a TMJ flare-up.
Understanding what causes your TMJ to flare up is the first real step toward finding relief. It’s all about pinpointing the specific stressors that push your jaw system past its tipping point. This concept map gives a great visual of how different issues all lead to the same destination: jaw pain.
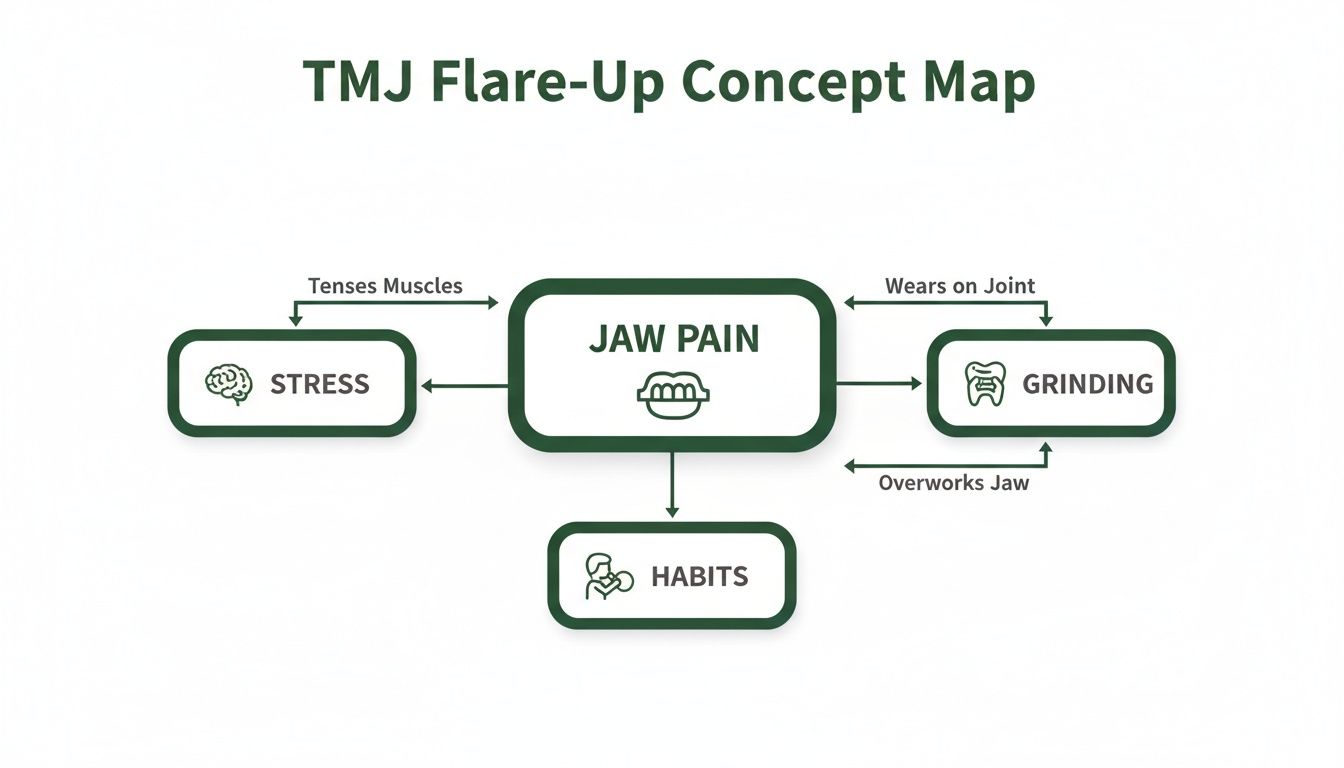
As you can see, emotional stress, physical grinding, and everyday habits are the main roads that converge, each contributing to muscle tension and joint inflammation in its own way.
The Cumulative Effect of Daily Stressors
It’s so important to realize that these triggers rarely act alone. Instead, they feed into each other, creating a cycle that can be incredibly difficult to break without the right help.
Picture this: a stressful day at work leads to unconscious jaw clenching. That tension carries over into the night, turning into teeth grinding while you sleep. By morning, your jaw muscles are already fatigued, making them far more vulnerable to irritation from something as simple as chewing a piece of gum.
A flare-up isn't a sign of weakness; it's a direct physiological response to sustained pressure. The muscles in your jaw can generate incredible force, and when that force is constant and uncontrolled, pain and dysfunction are the inevitable results.
This compounding effect is why your pain can feel so unpredictable. The triggers build up silently in the background until one minor action becomes the final straw. Recognizing these patterns is crucial, as many common symptoms of temporomandibular joint dysfunction go beyond the jaw itself, often showing up as headaches, earaches, and persistent neck tension.
Your Path to Identifying Triggers
The key to managing flare-ups is becoming an expert on your own body. For a quick overview of what to look for, this table breaks down the most common culprits.
Quick Guide to Common TMJ Flare Up Triggers
This table provides a quick summary of the primary causes behind TMJ flare-ups, helping you instantly identify potential sources of your jaw pain.
| Trigger Category | Common Examples | How It Strains the Jaw |
|---|---|---|
| Emotional Stress | Anxiety, frustration, high-pressure deadlines | Leads to unconscious jaw clenching and muscle tightening. |
| Parafunctional Habits | Teeth grinding (bruxism), nail-biting, chewing on pens | Creates excessive, non-functional force on the teeth and jaw joints. |
| Dietary Choices | Chewy foods (bagels, steak), hard foods (nuts, ice) | Forces the jaw muscles to work overtime, causing fatigue and strain. |
| Poor Posture | "Tech neck," slouching at a desk, cradling a phone | Pushes the jaw and head forward, straining the neck and jaw muscles. |
| Physical Strain | Intense workouts, yawning too wide, dental procedures | Can overextend or fatigue the jaw muscles and ligaments. |
By becoming more aware of these categories, you can start connecting the dots between your daily life and your jaw pain.
To get started, try keeping a simple journal for a week or two—it can reveal some powerful insights. Whenever your pain spikes, make a quick note and consider these factors:
- Emotional State: Were you feeling anxious, stressed, or frustrated?
- Dietary Choices: Did you eat anything particularly hard, chewy, or tough?
- Physical Activities: Were you slouching at your desk or engaging in intense physical activity?
- Sleep Quality: Did you wake up with a tight jaw or headache?
This simple act of observation empowers you to see the patterns for yourself and begin making small but meaningful changes that can lead to significant relief.
The Hidden Link Between Stress and Teeth Grinding

When it comes to TMJ pain, two factors often team up to create a powerful, destructive duo: emotional stress and nighttime teeth grinding. These aren’t just separate problems. They’re deeply connected forces that can trap you in a vicious cycle of tension and pain.
Getting to the bottom of this link is the first step in figuring out what causes TMJ to flare up for so many people.
Think about what happens when you’re stressed—a looming deadline, a financial worry, a tough conversation. Your body instantly kicks into "fight or flight" mode. It's an ancient survival instinct that floods your system with stress hormones like cortisol and adrenaline.
One of the first things to happen is involuntary muscle tension. Your body braces for a threat, and the muscles in your shoulders, neck, and—most importantly—your jaw tighten up. This isn't a conscious choice; it's a hardwired reflex.
How Stress Translates to Physical Pain
When stress becomes a constant companion, those jaw muscles never really get a break. They stay in a state of low-grade contraction, almost like a fist that’s always clenched.
This constant tension is a direct line to:
- Muscle Fatigue: Overworked muscles get exhausted and weak, creating a dull, aching pain that can radiate across your face and head.
- Inflammation: The nonstop strain triggers inflammation in the surrounding tissues, which adds swelling and sensitivity to the mix.
- Trigger Points: Tiny, painful knots of tight muscle fibers can form, sending pain to other areas and causing headaches or earaches.
This is exactly why a stressful week at work so often ends with a miserable TMJ flare-up. The emotional weight you carry all day physically lands right in your jaw, setting the stage for pain and dysfunction.
Your nervous system interprets emotional stress as a physical threat, and your jaw muscles respond by getting ready for a fight. Over time, this constant state of high alert simply wears down the entire jaw system.
And that daytime tension doesn't just disappear when you go to bed. It often spills over into your sleep, paving the way for an even more destructive habit.
The Destructive Force of Nighttime Grinding
All that tension you build up during the day has to go somewhere. For many people, it comes out at night through sleep bruxism, or nighttime teeth grinding. While you’re completely asleep and unaware, your jaw muscles can clamp down with incredible force, grinding your teeth together with pressure that far exceeds normal chewing.
This habit is a massive trigger for TMJ flare-ups because it puts the jaw joints and muscles under hours of intense, damaging strain. It’s not just about waking up with a sore jaw, headaches, and sensitive teeth; it also wrecks the restorative stages of your sleep. You can wake up feeling like you ran a marathon overnight, with your jaw taking the brunt of it.
It's a huge problem. The overlap between bruxism and TMD is significant—some studies show it skyrockets to 70% in North America. Considering TMJ disorders affect roughly 12% of the U.S. population (around 35 million people), bruxism could be the hidden culprit behind a massive number of those painful flare-ups.
This is where the cycle really locks in: stress leads to clenching, clenching leads to grinding, and grinding causes pain and poor sleep—which, of course, just ramps up your stress levels. Our guide on how to stop teeth grinding at night offers more strategies to break this pattern.
The key is to see stress and bruxism not as symptoms to endure, but as treatable root causes. Addressing them head-on is the only way to find a path to lasting relief.
How Everyday Habits Can Provoke Jaw Pain

While big-picture issues like stress or teeth grinding get most of the attention, it’s often the small, repetitive habits woven into our daily lives that keep TMJ pain going. These actions seem harmless on their own, but they add up, slowly pushing your jaw muscles and joints to a breaking point.
The good news is that once you start looking for these hidden triggers, you can make simple changes that bring incredible relief. It’s all about becoming a detective of your own daily routine.
Your Posture and Its Impact on Your Jaw
Think of your head as a bowling ball. When your posture is good, it’s balanced perfectly on top of your neck and shoulders. But when you slump forward, your neck and shoulder muscles have to work overtime just to keep it from falling.
This is exactly what happens with “tech neck.” As you lean forward to look at a phone or computer, that constant strain doesn’t just stay in your neck—it travels straight up to your jaw. The tension pulls your lower jaw backward, putting your TMJ under constant, low-grade stress.
Your sleeping position matters, too. Sleeping on your stomach forces your head to one side for hours, twisting your neck and creating an imbalance in your jaw joints. Even side-sleeping without the right pillow support can let your head droop, leading to the same kind of strain.
Your jaw joint doesn’t exist in isolation. It's the endpoint of a kinetic chain that starts in your upper back and neck. Poor posture essentially creates a constant, low-grade tug-of-war on your jaw muscles all day long.
The Food You Eat and the Strain It Creates
Sometimes, it’s not what you eat, but the mechanical effort it takes to eat it. Your jaw muscles are powerful, but they aren't meant for a non-stop workout. Foods that are overly hard, chewy, or tough can easily push them past their limit, triggering a painful flare-up.
This is why a simple lunch can sometimes turn into an afternoon of throbbing jaw pain. Your muscles have simply been overworked.
Watch out for these common culprits:
- Chewy Breads and Bagels: Their dense texture demands a lot of grinding, which can quickly exhaust your jaw muscles.
- Tough Meats: A piece of jerky or a tough steak forces your jaw to work much harder than it’s designed to.
- Hard Foods: Chewing on ice, hard candies, or even some nuts can place sudden, intense pressure on your jaw joints.
- Large Bites: Opening your mouth wide for a big sandwich or a whole apple can overstretch the joint and strain the ligaments that support it.
Being mindful of food textures—and maybe swapping for softer options when your jaw is already feeling sensitive—can make a huge difference.
Unconscious Habits That Sabotage Your Jaw
Beyond posture and diet, a whole category of triggers comes from using your jaw for things other than talking or eating. We call these parafunctional habits, and they’re especially sneaky because most of us do them without even realizing it.
These habits introduce unnatural, repetitive forces that your jaw system simply isn't built to handle. A few of the most common ones include:
- Nail-Biting: This habit forces your jaw into an awkward forward position and puts uneven pressure on your front teeth.
- Constant Gum Chewing: Think of it like sending your jaw muscles to the gym for hours without a rest day. It leads to classic overuse and fatigue.
- Using Teeth as Tools: Opening a package, cutting tape, or holding pins with your teeth places unpredictable and often damaging forces on your jaw joints.
- Resting Your Chin on Your Hand: This common desk posture shoves your jaw sideways, compressing one joint while overstretching the other.
Stress often acts like gasoline on the fire, turning these little habits into go-to coping mechanisms. In fact, research shows that nearly 30% of people globally are affected by TMD, and the most common type is muscle-related pain (37.2%), which is frequently sparked by these very stress-induced behaviors. You can discover more from the research about how stress fuels these TMJ triggers.
Learning to spot these habits is the first step. The next is consciously replacing them with healthier ones to break the pain cycle for good.
Of course. Here is the rewritten section, crafted to sound completely human-written and natural, following all your provided instructions and examples.
When the Joint Itself Is the Problem
While habits and stress are huge factors, sometimes the real answer to "what causes TMJ to flare up?" lies in the physical structure of your jaw joint. Think about it: if the joint is already unstable because of an old injury, an internal misalignment, or a degenerative condition, it's going to be far more vulnerable to painful episodes.
It helps to imagine the TMJ like a simple door hinge. When it’s perfectly aligned and well-oiled, the door swings smoothly without a sound. But what happens if someone slams into the door, bending the hinge? Or if it starts to rust over time? Even normal use will cause squeaking, grinding, and eventually, a total breakdown. Your jaw works on the same principle.
The Long Shadow of Jaw Injuries
Direct trauma is one of the clearest paths to structural TMJ problems. A blow to the face during a soccer game, a bad fall, or a car accident can have consequences that show up years down the road. Whiplash is a perfect example—the violent snapping motion of the head can easily stretch or tear the delicate ligaments that are supposed to keep the jaw joint stable.
Even an injury that felt minor at the time can lay the groundwork for future flare-ups. The initial damage might create a subtle, chronic instability that your jaw muscles have to work overtime to compensate for, leading to constant fatigue and inflammation.
Understanding the Slipped Disc in Your Jaw
Tucked inside your jaw joint is a small, flexible piece of cartilage called the articular disc. Its whole job is to act like a tiny shock absorber, letting the bones glide smoothly when you talk or chew. When everything is working right, this disc stays perfectly positioned right where it needs to be.
But if it gets damaged from an injury or chronic strain, this little cushion can slip out of place. This is a condition we call disc displacement.
Think of it like a pillow that's supposed to stay centered on a chair. If it slides forward, sitting down becomes awkward and uncomfortable. Disc displacement is the same idea—the jaw's "cushion" has moved, causing that painful clicking, popping, or even a locked jaw.
This isn't just a minor issue; it's a significant structural problem. Research shows that trauma can trigger these kinds of TMJ flare-ups years later, with studies finding disc displacements in a staggering 41.1% of TMD patients. In the U.S., where about 1 in 12 adults struggles with this condition, injuries like whiplash (which happens in 10-20% of car accidents) are a major culprit. You can dig into more data on the global prevalence of TMJ disorders to see just how common this is.
When Arthritis Sets in the Jaw Joint
Just like your knees or hips, the TMJ isn't immune to inflammatory conditions like osteoarthritis or rheumatoid arthritis. These diseases cause the protective cartilage inside the joint to wear down and deteriorate over time.
As that cartilage disappears, the bones can start grinding directly against each other. This friction leads to a grating sensation, stiffness, and chronic, nagging pain. This breakdown fundamentally changes how your jaw works, creating an environment where flare-ups become more frequent and much more severe.
When the joint's actual structure is compromised, just managing symptoms with heat packs and soft diets won't be enough for lasting relief. At this point, treatment has to shift from simply calming down the muscles to actively repairing and stabilizing the joint itself. This is where advanced non-surgical options, like regenerative therapies, come in. They are designed to address these root structural problems, helping your body heal damaged tissue and restore true, lasting function.
Moving Beyond Pain with Advanced Non-Surgical Treatments
Knowing what triggers a TMJ flare-up is one thing, but the real goal is to move beyond just managing pain and start truly healing. The good news? Modern treatment has evolved far beyond a simple night guard or pain medication. The focus now is on retraining your neuromuscular system and repairing joint damage at the source—all without invasive surgery.
This is a complete shift in thinking. Instead of just quieting symptoms, we can target the root functional problems, whether they’re caused by muscle habits, joint damage, or system-wide stress. This integrated approach combines specialized physical therapy for your face with your body's own incredible healing power.
Retraining Your Jaw with Orofacial Myofunctional Therapy
One of the most powerful ways to break the cycle of TMJ pain is through Orofacial Myofunctional Therapy (OMT). You can think of it as physical therapy designed specifically for your mouth, face, and jaw. It’s a series of targeted, painless exercises that correct poor muscle habits you might not even realize you have.
An OMT program helps you:
- Establish Proper Tongue Posture: This teaches your tongue to rest gently on the roof of your mouth, which naturally supports the jaw and encourages nasal breathing.
- Correct Swallowing Patterns: It re-patterns your swallow so the tongue pushes up against the palate instead of forward against your teeth, which dramatically reduces strain on the jaw.
- Improve Lip Seal: This ensures your lips stay comfortably closed at rest—a crucial component for proper jaw alignment and nasal breathing.
By retraining these foundational functions, OMT helps your jaw find its natural, relaxed resting position. This takes a huge amount of pressure off the TMJ, allowing overworked muscles to finally let go and inflammation to calm down. It’s all about building a stronger, more efficient foundation for long-term joint stability.
The Power of Correct Breathing
It might sound almost too simple, but how you breathe has a massive impact on your jaw. Chronic mouth breathing forces the jaw into a strained, open position and is often tied to the "fight or flight" stress response that fuels clenching and grinding.
Specialized breathing exercises, like those taught in the Buteyko method, focus on retraining your body to breathe calmly and efficiently through your nose. Nasal breathing does more than just filter and warm the air; it helps activate the parasympathetic nervous system—your body’s "rest and digest" mode.
Shifting from mouth breathing to nasal breathing is like flipping a switch from a state of high alert to one of deep calm. This simple change can dramatically reduce the systemic stress that causes unconscious muscle tension in your jaw, neck, and shoulders.
Sparking Natural Healing with Regenerative Medicine
Sometimes, the joint itself has sustained physical damage, like a displaced disc or arthritic changes. In these cases, we need to go beyond retraining muscles and actively help the joint structure repair itself. This is where regenerative treatments come in, using your body’s own healing agents to rebuild damaged tissue.
Two of the leading options are:
- Prolotherapy: This involves injecting a natural solution (like dextrose) into the weakened ligaments surrounding the jaw joint. This creates a mild, controlled inflammation that signals your body to flood the area with growth factors. It’s a powerful way to kickstart your natural healing response, strengthening and tightening ligaments to restore stability.
- Platelet-Rich Fibrin (PRF): This treatment uses a concentration of platelets and growth factors taken from a small sample of your own blood. When this PRF matrix is introduced into the TMJ, it acts like a biological scaffold, stimulating the regeneration of cartilage, ligaments, and other tissues. It’s like giving your body a supercharged toolkit to repair itself from the inside out.
These therapies aren’t a temporary patch; they're designed to genuinely heal damaged structures. You can learn more about how regenerative medicine for joint pain offers a path to recovery without surgery.
By combining these advanced treatments with functional therapies like OMT, we can address every facet of your TMJ disorder—from muscle habits to joint integrity—for comprehensive and lasting relief.
Time to Call a Professional? When Jaw Pain Warrants an Expert Look
While at-home remedies and self-care can be a great first line of defense for minor jaw discomfort, they aren't always enough. Knowing when to graduate from self-care to a professional evaluation is the key to getting real, long-term relief. Pushing through persistent symptoms can often let a small problem grow into a much bigger one.
So, when is it time to pick up the phone? Certain red flags are your body's way of telling you the issue is more than just a tired muscle and needs a much closer look from a specialist.
Don't Ignore These Red Flags
Your body is pretty good at telling you when something is seriously off. If you’re experiencing any of the following, it’s a clear signal that a professional evaluation for your jaw pain is in order:
- A Locked Jaw: This is a big one. If your jaw ever gets stuck open or shut, it points to a significant problem inside the joint itself that needs immediate attention.
- Pain That Won’t Quit: Aches that hang around for more than a few days, or pain that consistently gets in the way of eating, talking, or sleeping, isn't normal. This kind of chronic pain usually means there's an ongoing inflammatory or structural issue.
- Trouble Chewing: Finding yourself avoiding your favorite foods because chewing has become too painful or difficult is a major sign that your jaw function is compromised.
- Constant Clicking or Grating: An occasional, quiet pop might not be a concern. But a loud, painful click or a grinding, sandy sensation usually means the disc inside your joint is out of place or you're dealing with arthritic changes.
Think of these symptoms as your body's check-engine light. You can ignore it for a little while, but you risk turning a fixable issue into a major breakdown. A professional diagnosis is like plugging into the diagnostic computer to find the exact error code.
What a Professional Evaluation Looks Like
A thorough assessment isn't just about zeroing in on your jaw. It’s a deep dive designed to finally answer the question: what’s causing my TMJ to flare up? A specialist will look at the entire system—your bite, your muscles, your joints, your posture, and even the way you breathe.
This detailed exam is the first and most important step toward a treatment plan that’s actually built for you. By pinpointing the true source of your pain, you can stop chasing temporary fixes and start the journey toward a life without pain. If your symptoms are holding you back, don't wait. Schedule a consultation to get the clear answers and effective solutions you deserve.
Common Questions About TMJ Flare-Ups
If you're dealing with TMJ pain, you probably have a lot of questions. It's a complex issue, and finding clear answers can be tough. Let's walk through some of the most common concerns we hear from patients to help you better understand what's happening and what your next steps might be.
How Long Does a TMJ Flare-Up Last?
There’s really no one-size-fits-all answer here. A flare-up can last anywhere from a few hours to several weeks, and it often comes down to the trigger. For instance, if you strained your jaw eating something tough or chewy, the pain might be gone in a day or two.
But if the flare-up is tied to a bigger issue, like a period of intense stress causing you to grind your teeth all night, that discomfort can stick around for much longer. The real takeaway is this: if your pain lasts for more than a week or keeps coming back, it’s a clear signal that a deeper, underlying problem needs to be addressed by a professional.
Can My Bite or Recent Dental Work Trigger a Flare-Up?
Yes, absolutely. The way your teeth come together—what we call your occlusion—is a huge piece of the puzzle. If your bite is even slightly off, it forces your jaw muscles and joints into a strained, unnatural position every single time you close your mouth. Over time, that constant imbalance is a major reason for what causes TMJ to flare up.
Similarly, extensive dental work can easily set off a flare-up. Holding your mouth wide open for a long procedure can overstretch the joint. Even something as small as a new filling or crown that changes your bite ever so slightly can be enough to irritate an already sensitive system.
A proper TMJ evaluation always looks at the bigger picture. It's not just about the joint itself; it’s about the complex relationship between your teeth, muscles, airway, and bones. Finding and correcting these functional imbalances is often the key to lasting relief.
Is a Night Guard the Only Solution for Teeth Grinding?
A custom night guard is an essential tool, but it’s more of a shield than a true solution. It does a fantastic job of protecting your teeth from the incredible forces of grinding, preventing cracks and wear. What it doesn't do is stop the muscle activity that causes the grinding in the first place.
A truly effective treatment plan goes deeper to address why you're grinding. This usually means a multi-faceted approach, including:
- Orofacial Myofunctional Therapy to retrain the muscles of your face and mouth.
- Stress management techniques to help calm your nervous system.
- Breathing exercises to improve airway function and sleep quality.
Think of the night guard as a critical part of the team, but it works best when it's part of a bigger strategy that gets to the root cause of the problem.
Are My Headaches and Ear Pain Actually Connected to My Jaw?
Definitely. Headaches and ear pain are two of the most common symptoms we see in people with TMJ disorders. Your main chewing muscles are large and fan out across your temples. When those muscles get overworked and inflamed from clenching, the pain often radiates upward, feeling just like a persistent tension headache.
The link to ear pain is all about anatomy. Your temporomandibular joint is located right in front of your ear canal. When that joint gets inflamed, the swelling can put pressure on the surrounding ear structures. This can lead to earaches, a feeling of fullness, or even ringing in the ears (tinnitus). By resolving the jaw problem, we often see these related symptoms clear up, too.
At Pain and Sleep Therapy Center, we specialize in getting to the root cause of your jaw pain. We develop personalized, non-surgical treatment plans designed to restore function and bring you lasting comfort. If you're ready to move beyond temporary fixes, we invite you to explore our unique approach to TMJ relief.





