If you’re dealing with a clicking jaw, relentless headaches, and facial pain, the biggest question on your mind is probably a simple one: how long is this TMJ pain going to last?
There's no single, straightforward answer, but here’s a good rule of thumb. An acute, or short-term, TMJ flare-up often gets better on its own within a few days to several weeks. The real trouble starts when the underlying problems aren’t fixed. If that’s the case, the pain can dig in and become a chronic issue, sticking around for three to six months—or even longer.
Your Guide to the TMJ Pain Recovery Timeline

Figuring out your personal recovery timeline starts with understanding that TMJ pain isn't a one-size-fits-all problem. How long it lasts really depends on whether your pain is acute (a temporary flare-up) or has settled in for the long haul and become chronic.
Think of it like a sprained ankle. A minor twist might feel better after a few days of rest and ice. But if you’ve badly torn a ligament, you'll need a structured recovery plan with physical therapy to heal properly and avoid re-injury down the road. TMJ pain works in a very similar way.
Acute vs. Chronic: A Timeline Comparison
A temporary flare-up from a stressful week of clenching your teeth might fade away with some simple self-care. But persistent, nagging pain that stems from a deeper issue—like a misaligned bite, joint inflammation, or even a hidden airway problem—is not going to disappear on its own.
This guide will break down all the things that influence your recovery timeline, from the root causes to your treatment choices, giving you a much clearer roadmap. We'll look at why some cases resolve in a flash while others linger, and explain why getting to the real cause of the pain is the most important first step toward feeling better, faster.
The key takeaway is that the duration of TMJ pain is not random. It is directly linked to the underlying cause and the effectiveness of the treatment in addressing that specific cause.
So, let's take a quick look at the differences between acute and chronic TMJ pain. This will help you get a better sense of where you might fall on the spectrum.
TMJ Pain Timelines at a Glance
This table offers a clear side-by-side comparison to help you understand the two main types of TMJ pain.
| Characteristic | Acute TMJ Pain | Chronic TMJ Pain |
|---|---|---|
| Typical Duration | A few days up to a few weeks. | Persists for more than 3-6 months. |
| Common Causes | Stress, a temporary injury, or extensive dental work. | Underlying structural issues, arthritis, or central sensitization. |
| Symptoms | Sharp, localized pain; temporary clicking or popping. | Dull, aching pain; constant headaches; limited jaw movement. |
| General Outcome | Often resolves with self-care and conservative measures. | Requires a specialized diagnosis and a root-cause treatment plan. |
Understanding this distinction is so important. An approach that works for a short-term flare-up is almost never enough to fix a deep-seated, chronic condition. By figuring out the true nature of your pain, you can seek the right level of care and set realistic expectations for your recovery.
How Long Does TMJ Pain Last? Understanding Acute vs. Chronic Timelines
To really get to the bottom of the question, "How long does TMJ pain last?", we first need to understand that TMJ pain comes in two main flavors: acute and chronic.
Think of acute TMJ pain as a sudden, blaring fire alarm. It’s an immediate, often sharp signal that goes off because of a specific event—maybe you had a week of intense, stress-fueled clenching, spent a long time in the dentist's chair with your mouth wide open, or took a direct hit to the jaw. This kind of pain is your body’s direct and immediate response to a recent problem.
Chronic TMJ pain, on the other hand, is much more like faulty wiring running through the entire building. The alarm just won't shut off. The pain sticks around long after a normal healing period, which is typically about three to six months. It becomes a constant, nagging presence or a frustrating problem that keeps coming back.
This shift from a temporary alarm to a persistent state of alert isn’t just about the jaw joint itself. It often involves a fundamental change in how your nervous system is processing pain signals altogether.
The Shift from a Simple Warning to a Chronic Condition
When pain becomes chronic, the nervous system can get stuck in a state of high alert, a condition known as central sensitization. In this state, your brain and spinal cord start to amplify pain signals. It’s like turning the volume knob on a stereo all the way up—even the quietest sounds become overwhelmingly loud.
This means that things that shouldn't hurt, like gently touching your face or chewing soft food, can suddenly feel excruciating. It’s a huge reason why treatments that might work for an acute flare-up—like a simple painkiller or a generic, over-the-counter night guard—often fail when you're dealing with a chronic condition. They might muffle the alarm for a bit, but they do absolutely nothing to fix the faulty wiring.
A chronic TMJ condition isn't just a "sore jaw" anymore. It becomes a complex neurological issue where the pain signaling system itself has gone haywire, and that requires a much more sophisticated approach to reset it.
Why a One-Size-Fits-All Approach Fails
This difference between acute and chronic pain is exactly why a one-size-fits-all approach is so ineffective. Treating chronic TMJ pain means we have to look past the immediate symptoms and dig for the underlying issues that are driving the pain.
What causes an acute problem to spiral into a chronic one? A few key factors are often at play:
- Unresolved Structural Issues: A displaced disc in the jaw or degenerative joint disease simply won't heal with a "wait and see" approach.
- Perpetuating Habits: If you're constantly grinding your teeth (bruxism) or have poor posture, you're essentially re-injuring the jaw muscles and joints day after day.
- Co-existing Conditions: Problems like sleep apnea or systemic inflammation can pour fuel on the fire, creating a vicious pain cycle that prevents recovery.
The good news? Even when TMJ pain becomes chronic, it's rarely a life sentence. Research actually shows that for most people, the condition comes and goes rather than being constant. One study that followed patients for eight years found that most cases of TMJ pain either resolved on their own or recurred periodically instead of persisting without a break. In fact, only about 15% of people who seek care for TMJ pain go on to develop a truly chronic, persistent condition. You can read more about these important TMJ recovery statistics.
Understanding whether your pain is an acute event or a chronic condition is the first, most important step. It helps set realistic expectations for your recovery and points you toward a treatment plan that addresses the real source of the problem, not just the symptoms.
Key Factors That Influence Your TMJ Recovery Time
Have you ever wondered why a friend's TMJ pain disappeared in a couple of weeks, but yours has stuck around for months? It’s not just a matter of luck. The answer lies in a few key factors that create your unique recovery timeline. How long your pain lasts is a direct reflection of what's happening inside your body.
Understanding these influences is the first real step toward an effective treatment plan. Instead of just chasing symptoms, a root-cause approach digs into the "why" behind your pain, which can dramatically shorten your path to feeling better.
The Root Cause Dictates the Timeline
The single biggest factor that determines how long recovery will take is the underlying cause of your TMJ disorder (TMD). A problem that starts in the muscles has a completely different timeline than one rooted in the joint itself.
Muscular Pain: This is usually the quickest to resolve. If your pain is coming from overworked or tense jaw muscles—maybe from stress or a recent dental procedure—it can often improve within a few days to a few weeks with the right self-care and relaxation techniques.
Joint Inflammation (Arthritis): When inflammation is the main issue, recovery takes a bit longer. The goal here is to manage the inflammatory response, a process that can take several weeks or even months of consistent treatment.
Disc Displacement: If the small, shock-absorbing disc inside your jaw joint has slipped out of place, the timeline gets more complex. Recovery focuses on either recapturing the disc or helping the joint adapt to its new position, which can span several months and requires professional guidance.
Think of it like a problem with your car. A flat tire (a muscular issue) is a pretty quick fix. But engine trouble (a joint issue) needs a skilled mechanic and a much more involved repair process.
Daily Habits That Extend Pain Duration
Your daily habits can either help you heal or constantly sabotage your progress, creating a frustrating cycle of pain that never seems to end. Many people don't even realize they're contributing to their own prolonged TMJ pain with seemingly harmless routines.
One of the most common culprits is poor posture. That "forward head posture" so many of us have from sitting at a desk puts constant strain on the neck and jaw muscles, preventing them from ever fully relaxing and healing. Simple habits like chewing gum, biting your nails, or resting your chin in your hand can also keep that muscle tension going.
Another huge factor is bruxism—the medical term for chronic teeth grinding and clenching. This often happens unconsciously while you sleep, overloading the jaw joints and muscles night after night. It's like re-injuring yourself every single night, making lasting relief impossible without addressing it. If this sounds familiar, you might want to learn more about the common triggers for TMJ flare-ups to see what your personal patterns are.
The Role of Co-Existing Conditions
Finally, your overall health plays a massive role. TMJ pain rarely exists in a vacuum. It's often tangled up with other health conditions that can complicate and prolong the recovery process.
Certain factors act as predictors for whether TMJ pain will become a persistent, long-term issue. Research highlights that the number of pain sites, the intensity of the pain, and the presence of co-existing health conditions are significant indicators.
For example, conditions like fibromyalgia can amplify pain signals all over the body, making TMJ symptoms feel more intense and last longer. Even more directly, undiagnosed sleep apnea is a powerful driver of chronic TMJ pain. The nightly struggle to breathe often leads to intense jaw clenching as the body tries to force the airway open, creating a vicious cycle of poor sleep and jaw pain.
Studies have confirmed just how critical these perpetuating factors are. Globally, while 3.6% to 7% of people seek treatment for TMD, this number spikes to 18% in women between 25 and 44. Things like pain that gets worse when you eat tough foods or having multiple sore spots around your jaw can signal a higher risk for a longer recovery. A successful treatment plan absolutely must address this complete picture, not just the jaw itself.
Realistic Recovery Timelines for Different TMJ Treatments
So, how long does this actually take? That’s the big question.
When it comes to TMJ pain, there’s no single, one-size-fits-all answer. Your recovery timeline really depends on the treatment you’re getting. Thinking about it this way helps set realistic expectations from the start, making the whole healing process feel a lot less frustrating.
Just like you wouldn’t expect a badly sprained ankle to feel brand new overnight, real TMJ relief takes a bit of patience and consistency. The path you choose—from simple home care to more advanced therapies—will set the pace for your recovery.
Conservative and At-Home Care Timelines
For a mild, new flare-up, we often start with conservative, at-home strategies. These are simple, non-invasive things you can do right now to calm down an angry jaw joint and give overworked muscles a break.
- Soft Diet and Jaw Rest: Simply giving your jaw a vacation from hard, chewy foods can make a world of difference. Many people feel a noticeable improvement in just a few days to a week.
- Heat and Cold Therapy: Alternating between a warm compress on tight muscles and an ice pack on an inflamed joint can bring immediate, short-term relief. If you stick with it during a flare-up, you can seriously dial down your symptoms in under two weeks.
These are fantastic for managing temporary pain, but they’re band-aids. They don’t fix what’s actually causing the problem, which is why they aren’t a long-term solution for chronic TMJ issues.
Professional and Advanced Treatment Timelines
When TMJ pain just won’t quit, it’s a clear signal that something deeper is going on. This is where professional therapies come in. They’re designed to get to the root of the problem, leading to more predictable and lasting relief, even if the timeline is a bit longer.
Getting a good outcome really hinges on three things: figuring out the true cause, changing the daily habits that are contributing to it, and managing any other health conditions you might have going on.
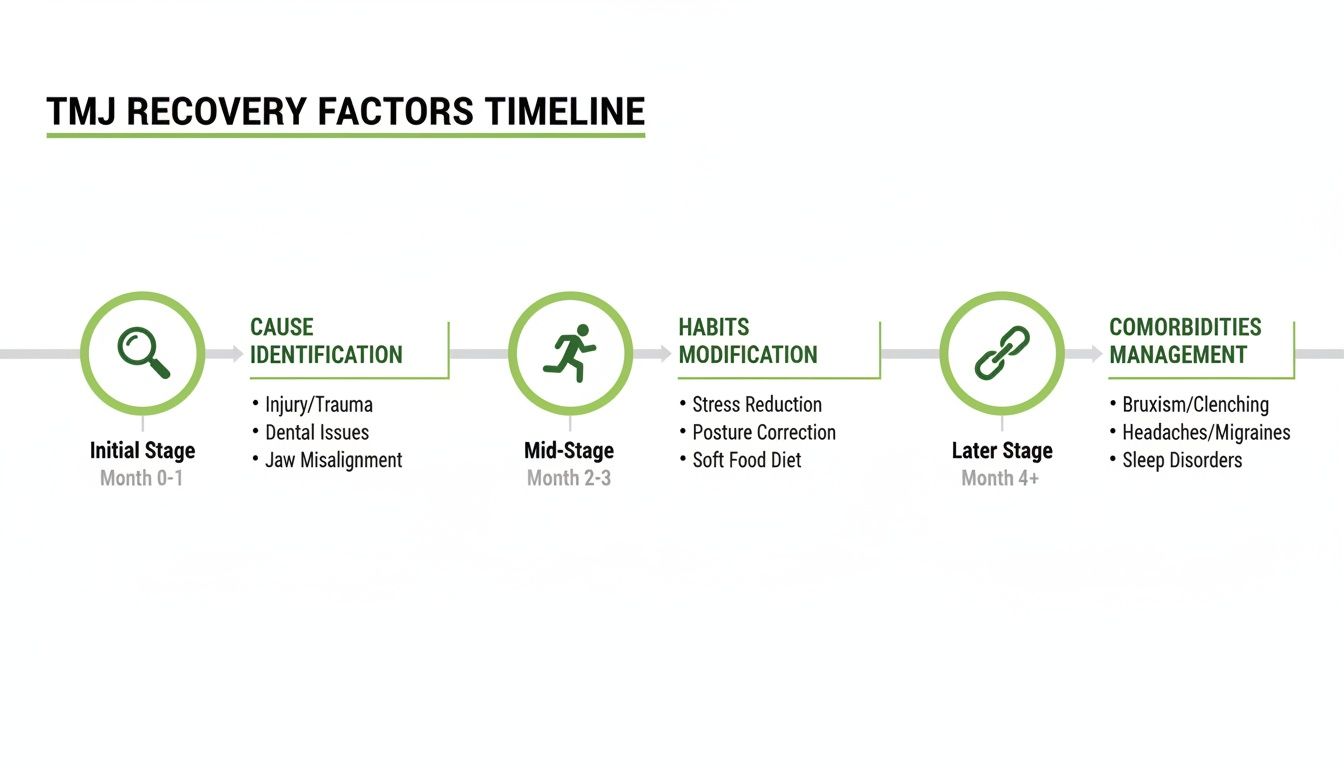
As you can see, getting these things in the right order—cause, habits, and related issues—is the key to a faster, smoother healing journey.
Custom Oral Appliances
A custom-fitted oral appliance (often called a splint) is a game-changer for many patients. Unlike the boil-and-bite guards you find at the drugstore, these are precision-made to decompress your jaw joint and help those constantly tense muscles finally relax.
Most patients tell us they feel initial relief from pain and headaches within the first few weeks of wearing their appliance consistently. But for the full effect—letting the bite and joint truly stabilize—it can take anywhere from 2 to 6 months as the muscles retrain and the inflammation finally calms down.
Orofacial Myofunctional Therapy
Think of this as physical therapy, but specifically for the muscles of your face, mouth, and tongue. It’s all about correcting poor muscle habits and posture that are feeding into your TMJ pain.
With a consistent routine of exercises, patients usually see real functional improvements, like smoother jaw movement and less clicking, within 1 to 3 months. The whole point is to build new, healthy muscle patterns that will keep your jaw stable for the long haul. If you want to see how this fits in with other approaches, you can learn more about the various TMJ treatment options we offer.
Regenerative Injection Therapies
Sometimes, the TMJ problem is actually damage inside the joint itself, like loose ligaments or worn-down cartilage. For this, regenerative treatments like Prolotherapy or Platelet-Rich Fibrin (PRF) can work wonders by kickstarting your body's own natural healing engine.
This typically involves a series of 3 to 6 injection sessions, spaced a few weeks apart. While you might feel some improvement early on, the real magic happens over time. Significant healing often takes 3 to 9 months as your body slowly builds new, healthy tissue. It’s an investment in a root-cause solution that leads to a much more predictable and permanent recovery.
How to Speed Up Your TMJ Recovery at Home

While getting the right professional care is crucial for complex TMJ problems, you have a surprising amount of control over your healing timeline right from home. It's about integrating a few simple, intentional habits into your day. These small changes can calm down irritated joints and muscles, which is a huge part of shortening your own personal answer to "how long does TMJ pain last?"
Taking these proactive steps can make a real difference, shortening your recovery and even making professional treatments more effective. When you become an active participant in your healing, you start to take back control from the pain.
Practice Mindful Jaw Relaxation
One of the most powerful things you can do is simply teach your jaw how to rest. So many of us hold tension in our jaw all day long without even realizing it, never giving those overworked muscles a chance to heal. The goal is to find a neutral, relaxed position and make it your default.
Try to maintain the "lips together, teeth apart" posture. Let your tongue rest lightly on the roof of your mouth, right behind your front teeth. This one small adjustment can break the cycle of constant muscle strain.
Consciously check in with your jaw a few times an hour. Are your teeth clenched? Is there tension? Just a few seconds of awareness can release hours of built-up strain, offering immediate relief and setting the stage for faster healing.
It might feel strange at first. Try setting a quiet reminder on your phone or putting a small sticky note on your computer monitor. Every time you notice it, take a slow breath and consciously let your jaw go slack. Before long, this relaxed state will start to feel normal.
Adopt an Anti-Inflammatory Diet
What you eat has a direct line to the inflammation levels in your body—and that includes your jaw joints. When your TMJ is flared up, it desperately needs a break from hard, chewy, or crunchy foods that force it to grind and work overtime.
Instead of fighting your way through a tough steak or a crusty piece of bread, give your jaw a vacation. Choosing softer foods reduces the mechanical stress on the joint, giving it the space it needs to finally calm down and heal.
Jaw-Friendly Food Swaps:
- Instead of: Bagels, steak, or raw carrots
- Try: Scrambled eggs, smoothies, yogurt, and well-cooked vegetables
- Instead of: Chewing gum or sticky candy
- Try: Soups, mashed potatoes, and soft fruits like bananas
By simply reducing your jaw's daily workload, you allow that inflammation to subside much more quickly, which directly shortens how long the pain sticks around. To learn more about managing symptoms yourself, take a look at our complete guide to effective TMJ home care strategies.
Make Simple Ergonomic Adjustments
Your environment can either be your ally or your enemy when it comes to TMJ recovery. Poor posture, especially the kind we fall into at our desks or even while we sleep, puts constant strain on our neck and jaw muscles, keeping us stuck in a cycle of pain.
Take a hard look at your workspace. Is your computer monitor at eye level? If it's too low, you’re likely leaning into a "forward head posture," which is a notorious contributor to both neck and jaw pain. An easy fix is to stack a few books under your monitor until your head can rest in a neutral, balanced position.
Your sleeping setup matters just as much. Sleeping on your stomach often forces your neck into a twisted position and puts uneven pressure on your jaw. Try to sleep on your back, or on your side with a supportive pillow that keeps your head and neck aligned. These small, consistent changes add up, reducing the daily strain that feeds the pain cycle and giving your body a real chance to heal.
When to See a Specialist for Your Jaw Pain
So, how do you know if your jaw pain is a fleeting annoyance or a sign of something more serious? While a lot of minor flare-ups will fade with a little self-care, some symptoms are your body’s way of waving a big red flag. Ignoring them can turn a solvable, short-term problem into a chronic one, stretching out your recovery for months or even years.
The first step is simply to listen to your body. If the pain just won't quit after a few weeks of trying home remedies, that's a pretty clear signal that the real cause hasn't been addressed.
The Warning Signs You Shouldn't Ignore
Think of these symptoms as the "check engine" light for your jaw. If any of them sound familiar, it's time to get a professional diagnosis to figure out what's really going on and how long your TMJ pain might last.
- Your jaw locks up: It gets stuck open or shut, even for a moment.
- It’s hard to function: You're genuinely struggling to chew, talk, or open your mouth wide.
- The pain is spreading: You have constant, intense headaches or earaches that are clearly connected to your jaw issue.
- There are noises with pain: Any clicking, popping, or grinding sound that comes with discomfort often points to a problem inside the joint itself.
Pushing through these symptoms is like driving your car while that check engine light is flashing—it almost never ends well. A specialist with dedicated training in orofacial pain can do more than just quiet the symptoms; they can pinpoint the true source of the problem and map out a clear path to lasting relief.
The real goal of seeing a specialist isn't just to stop the pain you have now. It's to figure out why it's happening and prevent it from coming back, breaking the cycle of chronic pain for good.
It's true that a huge number of Americans will have some kind of TMJ symptom in their lifetime. But far fewer develop a persistent problem. While an estimated 20 million adults deal with active TMJ pain each year, only about 5.3 million of them seek help within the first 6 to 12 months. That delay can make a huge difference. The good news is that the outlook is great for people who get timely care. Chronic pain, meaning pain that lasts longer than 3-6 months, only affects about 15% of those who get treatment. You can read more about how TMJ disorders progress here.
Bottom line: if your jaw pain is getting in the way of your life, making a specialist appointment isn't an overreaction. It’s the most important step you can take toward getting your comfort and function back.
A Few Lingering Questions About TMJ Pain
Even with a clearer picture of recovery timelines, you probably still have a few specific questions floating around. We get it. Let’s tackle some of the most common ones we hear from our patients to help you know what to expect on your own healing journey.
Can TMJ Pain Just Go Away on Its Own?
Sometimes, yes. A mild case of acute TMJ pain, especially if it’s tied to a temporary trigger like a week of high stress, can absolutely resolve on its own. This kind of pain often fades within a few days to a couple of weeks with a little rest and some basic self-care.
But here’s the important part: if the pain is coming from an underlying structural problem—think arthritis, a misaligned bite, or a displaced disc in the joint—it's highly unlikely to just disappear. Waiting it out in these cases, unfortunately, can give a manageable issue the time it needs to turn into a chronic one.
How Long Does a Typical TMJ Flare-Up Last?
A TMJ flare-up is that lovely spike in your symptoms that comes out of nowhere. It can last anywhere from a few hours to several days. For more moderate cases, you might feel it lingering for up to two weeks.
The exact duration really depends on what kicked it off and how quickly you can respond with some supportive care. Common culprits include trying to eat something extra chewy, a bad night of teeth grinding, or even just a long appointment at the dentist. If you notice your flare-ups are happening more often, lasting longer, or feeling more intense, that’s a pretty clear signal that the underlying cause needs a professional look.
Think of a flare-up as your body’s way of saying the system is overloaded. The key to making them less frequent and severe is to consistently manage your triggers and address the root cause.
Will a Night Guard Actually Shorten My TMJ Pain?
A custom-fitted oral appliance from a TMJ specialist can make a world of difference in shortening how long your TMJ pain lasts. This is a far cry from the generic, over-the-counter guards that can sometimes make the problem worse. A custom device is designed with incredible precision to decompress your specific jaw joint, give tense muscles a chance to relax, and protect your teeth from grinding.
Many of our patients feel significant relief from their most disruptive symptoms, like headaches and muscle pain, within just a few weeks of wearing it consistently. This makes a custom appliance a true cornerstone of effective treatment. It provides the stability and rest your jaw needs to finally start healing, helping to stop acute pain from settling in for the long haul.
Is It Really Possible for TMJ Pain to Last for Years?
Unfortunately, yes. When the real root cause of a TMJ disorder isn't accurately diagnosed and properly treated, the condition can shift from an acute problem to a chronic one that sticks around for years. This is what happens when critical contributing factors get overlooked.
What kind of factors? We often see things like:
- Airway Issues: Undiagnosed sleep apnea can lead to some seriously intense nighttime clenching.
- Systemic Inflammation: Other health conditions can be secretly fueling inflammation in your jaw joints.
- Joint Degeneration: Structural damage inside the joint that has gone unaddressed for too long.
Getting an early and accurate diagnosis from a specialist is the single most effective way to break that pain cycle. By finding and treating the true source of the dysfunction, you can sidestep years of unnecessary discomfort and finally find relief that lasts.
At the Pain and Sleep Therapy Center, we specialize in root-cause diagnostics to create a clear and effective path to recovery, helping you find lasting relief from jaw pain. Schedule your consultation today and take the first step toward a pain-free life.





