If you're one of the millions struggling with jaw pain, clicking, or headaches, you know that finding effective relief can feel like an endless journey. The complex nature of Temporomandibular Joint (TMJ) disorders means that a one-size-fits-all approach often fails to deliver lasting results. The search for the best TMJ treatments is not just about masking symptoms; it's about understanding and addressing the root cause of your pain. From the way you breathe to the subtle mechanics of your bite, every element plays a critical role in jaw health and overall well-being.
This guide moves past temporary fixes and dives deep into the most innovative, evidence-informed therapies available today. We will explore a range of powerful, targeted solutions designed to restore function and eliminate discomfort for good.
You will learn about:
- Regenerative Therapies: How injections like Prolotherapy and Platelet-Rich Fibrin (PRF) can help rebuild damaged joint tissue.
- Neuromuscular Retraining: The role of specialized Physical Therapy and Orofacial Myofunctional Therapy in correcting harmful muscle patterns.
- Airway-Focused Solutions: The connection between breathing, sleep, and jaw pain, and how techniques like Buteyko Breathing can make a difference.
- Advanced Modalities: The benefits of non-invasive options like Cold Laser Therapy for reducing inflammation and promoting healing.
- Precision Diagnostics: Why accurate diagnosis using tools like CBCT scans is the essential first step toward effective treatment.
Whether you're dealing with a recent flare-up or chronic discomfort, this comprehensive roundup is designed to empower you with the knowledge needed to build a personalized roadmap to recovery. It will help you navigate your options and partner with specialists, like those at the Pain and Sleep Therapy Center, who utilize an airway-focused, interdisciplinary approach to reclaim a life free from jaw pain.
1. Physical Therapy & Myofunctional Therapy
Physical and Orofacial Myofunctional Therapy (OMT) is a specialized, exercise-based treatment that targets the root causes of TMJ disorders. Unlike passive treatments, this approach actively retrains the muscles of the mouth, face, and jaw to restore correct function, addressing issues like improper tongue posture, dysfunctional swallowing patterns, and compromised breathing mechanics.

The therapy involves a series of guided exercises performed both with a therapist and at home. The goal is to strengthen underdeveloped muscles and eliminate harmful compensatory habits that contribute to jaw pain, clicking, headaches, and even sleep-breathing disorders. This makes it one of the best TMJ treatments for long-term, sustainable relief.
Who Benefits from This Approach?
This therapy is highly effective for a wide range of patients. For instance, individuals with sleep apnea can improve airway patency through tongue positioning exercises, while those suffering from chronic tension headaches often find relief by learning jaw relaxation protocols and correcting forward head posture. For patients experiencing persistent muscle-related TMJ pain, specialized approaches like Myofascial Release Trigger Points are often incorporated into physical therapy programs.
Practical Tips for Success
To maximize the benefits of physical and myofunctional therapy, consistency is key.
- Create a Routine: Integrate exercises into your daily schedule, such as during work breaks or before bed.
- Stay Mindful: Pay attention to your jaw, tongue, and head posture throughout the day and make real-time corrections.
- Use Feedback: Practice exercises in front of a mirror or record yourself to ensure you are using the correct technique.
- Combine Techniques: Enhance your results by incorporating nasal breathing awareness and techniques like Buteyko breathing to optimize respiratory patterns.
By addressing the foundational mechanics of how your jaw, tongue, and facial muscles work together, physical and myofunctional therapy provides a powerful, non-invasive path toward lasting TMJ pain relief and improved overall function.
2. Prolotherapy (Proliferation Therapy)
Prolotherapy, also known as proliferation therapy, is a regenerative injection technique designed to stimulate the body's natural healing cascade within damaged TMJ structures. Unlike treatments that mask symptoms, prolotherapy targets the root cause of joint instability by strengthening weakened ligaments and tendons. The procedure involves injecting a mild irritant solution, typically dextrose, into the specific areas of injury or laxity.
This injection triggers a localized, controlled inflammatory response, which signals the body to recruit growth factors and build new, healthy connective tissue. Over a series of treatments, this process tightens and strengthens the ligaments, restoring stability to the jaw joint. This makes it one of the best TMJ treatments for addressing chronic clicking, popping, and hypermobility.
Who Benefits from This Approach?
Prolotherapy is particularly effective for individuals whose TMJ disorder stems from ligamentous laxity or chronic joint instability, often caused by injury or overuse. For example, a patient with a history of whiplash who experiences persistent jaw clicking and deviation may find that prolotherapy stabilizes the joint where other treatments have failed. It is also a valuable non-surgical option for those with joint hypermobility who need to restore structural integrity to prevent dislocations and reduce chronic pain.
Practical Tips for Success
To achieve the best possible outcomes with prolotherapy, patient commitment and proper aftercare are crucial.
- Complete the Full Series: A typical course involves 4-6 injection sessions. Do not stop early, even if you notice initial improvement, as full ligamentous strengthening takes time.
- Manage Post-Injection Care: Avoid aggressive jaw movements or hard-to-chew foods for 48 hours after each injection. Use ice for the first 24 hours to manage swelling, then switch to moist heat as needed for comfort.
- Stay Consistent with Therapy: Continue your physical or myofunctional therapy exercises concurrently. Strengthening the muscles while stabilizing the ligaments creates a comprehensive and durable result.
- Track Your Progress: Keep a detailed log of your pain levels, jaw sounds, and functional improvements between sessions. This data helps your provider tailor the treatment plan effectively.
By promoting the body's own regenerative capabilities, Prolotherapy offers a powerful solution for rebuilding joint stability and achieving long-term relief from TMJ-related pain and dysfunction.
3. Platelet-Rich Fibrin (PRF) Injections
Platelet-Rich Fibrin (PRF) is an advanced regenerative therapy that harnesses the body's natural healing capabilities to repair damaged TMJ tissues. This cutting-edge treatment uses concentrated platelets and growth factors isolated from a small sample of the patient's own blood. Unlike older methods, PRF creates a natural fibrin scaffold that slowly releases healing proteins over several days, promoting sustained tissue regeneration and reducing inflammation directly within the jaw joint.
The procedure involves a simple blood draw, spinning the blood in a centrifuge to separate the PRF, and then carefully injecting the concentrated biological material into the TMJ. This targeted approach stimulates the repair of cartilage and connective tissues, reduces pain, and improves overall joint function without introducing any synthetic materials or systemic drugs, making it one of the best TMJ treatments for those seeking a biological and minimally invasive solution.
Who Benefits from This Approach?
PRF injections are highly effective for patients with joint-based TMJ disorders, particularly those involving cartilage degeneration or inflammation. For instance, individuals diagnosed with TMJ osteoarthritis often see a reduction in pain and improved joint mobility, with some studies showing evidence of cartilage regeneration on follow-up imaging. Patients with chronic clicking and popping sounds due to internal derangement or those recovering from a traumatic jaw injury can also achieve significant functional improvement, often avoiding the need for more invasive surgical procedures.
Practical Tips for Success
To get the most out of your PRF treatment, proper preparation and aftercare are crucial.
- Hydrate Well: Drink plenty of water for 24 hours before your appointment to ensure a high-quality blood draw and optimal PRF yield.
- Avoid NSAIDs: Stop taking non-steroidal anti-inflammatory drugs (like ibuprofen) for about a week before and 2-3 weeks after your injection, as they can interfere with the body's natural healing response.
- Plan for Recovery: Apply ice for 20 minutes post-injection to manage swelling and stick to soft foods for 48-72 hours to allow the joint to rest.
- Follow the Protocol: PRF is often administered in a series of injections; be sure to schedule follow-up treatments as recommended by your provider for the best cumulative results.
By using your body’s own growth factors to heal from within, PRF injections offer a powerful, natural pathway to lasting relief from TMJ pain and restored jaw function.
4. Cold Laser Therapy (Low-Level Laser Therapy)
Cold laser therapy, also known as Low-Level Laser Therapy (LLLT), is a non-invasive treatment that uses specific wavelengths of light to penetrate deep into tissues without generating heat. This light energy stimulates cellular mitochondria, boosting the production of ATP (the energy currency of the cell). For TMJ disorders, this process helps reduce inflammation, alleviate pain, improve circulation to the joint, and accelerate tissue repair, making it one of the best TMJ treatments for acute pain and inflammation.
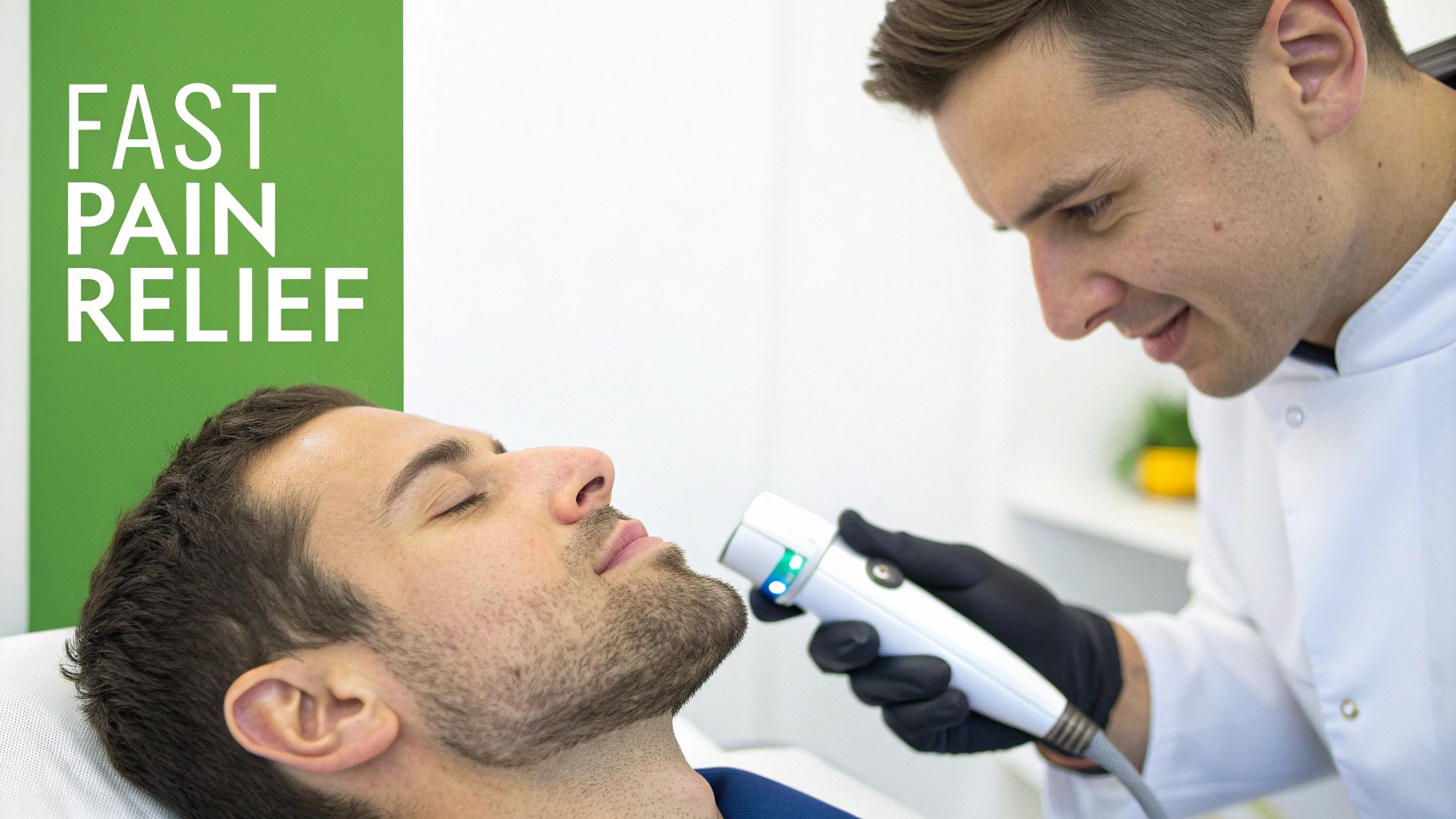
The treatment is painless, quick, and can be easily integrated into a broader therapeutic plan. By targeting the source of pain at a cellular level, LLLT helps to calm irritated nerves and relax tense jaw muscles, offering noticeable relief often within just a few sessions. This makes it an excellent complementary therapy to more foundational treatments like physical or myofunctional therapy.
Who Benefits from This Approach?
This therapy is particularly effective for patients experiencing acute TMJ flare-ups, providing rapid pain relief and reducing swelling. For instance, athletes with a jaw injury can use LLLT to speed up their return to competition. It's also beneficial for individuals with chronic tension headaches linked to myofascial pain, especially when combined with exercises to correct underlying biomechanical issues. Even post-surgical patients, such as infants after a frenectomy, can experience faster healing and reduced inflammation with targeted laser therapy.
Practical Tips for Success
To achieve the best outcomes with cold laser therapy, it should be part of a comprehensive strategy.
- Combine with Other Therapies: Use LLLT as an adjunct to myofunctional therapy and postural correction, not as a standalone cure. It addresses symptoms, while other therapies correct the root cause.
- Be Consistent: Schedule sessions consistently, such as once or twice a week, to build upon the therapeutic effects. Sporadic appointments are less effective.
- Track Your Progress: Keep a detailed pain log to monitor your symptoms and objectively assess your response to the therapy over time.
- Set Realistic Expectations: Discuss with your provider how LLLT fits into your overall treatment plan. While it offers significant relief, lasting success comes from correcting the biomechanical and functional issues contributing to your TMJ disorder.
5. Buteyko Breathing Technique
The Buteyko Breathing Technique is a specialized breathing retraining program designed to normalize dysfunctional breathing patterns, particularly chronic mouth breathing and hyperventilation. Developed by Dr. Konstantin Buteyko, this method teaches individuals to restore light, slow, and exclusively nasal breathing. This process helps rebalance blood gases, improve oxygen delivery to tissues, and calm the nervous system.
For TMJ disorders, correcting breathing is fundamental. Mouth breathing forces the jaw into a recessed, open posture, which strains the TMJ and associated muscles. The Buteyko method addresses this by re-establishing nasal breathing, which promotes proper tongue posture against the palate and a more stable, relaxed jaw position. This shift makes it one of the best TMJ treatments for addressing underlying airway issues that contribute to jaw pain.
Who Benefits from This Approach?
This technique is highly effective for a wide range of patients whose TMJ symptoms are linked to airway and breathing dysfunction. For example, individuals with sleep apnea can often reduce their apnea-hypopnea index (AHI) by restoring nasal breathing. Patients suffering from anxiety-related jaw clenching find that Buteyko’s focus on calming the nervous system through breath control significantly reduces their symptoms. It’s also invaluable for chronic mouth-breathers who experience TMJ clicking and tension, as the retraining directly resolves the dysfunctional habit.
Practical Tips for Success
To gain the most from the Buteyko method, consistent and mindful practice is essential.
- Establish a Routine: Dedicate specific times each day, such as morning, midday, and evening, to practice your breathing exercises.
- Prioritize Nasal Hygiene: Use a nasal saline rinse daily to ensure your nasal passages are clear and make nasal breathing easier to maintain.
- Track Your Progress: Keep a sleep diary to monitor objective improvements in snoring, sleep quality, and daytime energy levels.
- Practice Gradually: When performing breath-hold exercises, start slowly and avoid straining. The goal is gentle adaptation, not forced change.
- Integrate with Other Therapies: Combine Buteyko breathing with orofacial myofunctional therapy for faster and more comprehensive airway optimization.
By retraining your body’s most fundamental function, breathing, the Buteyko technique provides a powerful, non-invasive strategy to alleviate jaw strain, improve sleep, and achieve lasting relief from TMJ-related pain.
6. Oral Appliance Therapy (Custom Bite Splints & Sleep Position Devices)
Oral Appliance Therapy involves custom-fabricated devices, such as bite splints, night guards, and mandibular advancement devices (MADs), designed to address TMJ dysfunction. These appliances mechanically reposition the jaw and tongue to reduce muscle tension, prevent destructive habits like grinding and clenching, and improve airway patency during sleep. Unlike generic, over-the-counter options, custom devices are precisely molded to your anatomy, ensuring optimal fit and effectiveness.

This therapy serves a dual purpose: it protects your teeth from the significant damage caused by bruxism while simultaneously creating an ideal environment for inflamed TMJ structures to heal. By stabilizing the jaw in a therapeutic position, these appliances are a cornerstone of non-invasive care and are considered one of the best TMJ treatments for managing symptoms and promoting long-term joint health.
Who Benefits from This Approach?
This treatment is highly beneficial for patients with specific TMJ-related conditions. For instance, individuals with severe bruxism can achieve significant pain reduction while protecting their teeth from further wear. Many TMJ sufferers also experience bruxism, or teeth grinding. For those wondering how to stop grinding your teeth, various dental interventions and lifestyle changes can offer significant relief. Additionally, patients with sleep-breathing disorders may see improvements in their apnea-hypopnea index (AHI) scores using a mandibular advancement device, which gently moves the lower jaw forward to open the airway. Those with joint clicking and popping often find symptom resolution with stabilization splints that decompress the jaw joint.
Practical Tips for Success
To get the most from your oral appliance, adherence and proper care are essential.
- Be Consistent: Wear your device every single night. Irregular use can significantly diminish its therapeutic benefits.
- Allow for Adjustment: Give yourself a 2-4 week adjustment period to get used to the appliance before evaluating its full effectiveness.
- Schedule Follow-Ups: Your provider will need to make periodic adjustments to refine the fit as your jaw muscles relax and symptoms improve.
- Keep it Clean: Clean your device daily with a soft toothbrush and mild soap to prevent bacterial buildup.
- Combine Therapies: For superior long-term outcomes, coordinate the use of your appliance with a physical or myofunctional therapy program to retrain jaw muscles.
By providing mechanical support and promoting a healthier jaw position, custom oral appliances offer a powerful and personalized solution for managing pain, protecting teeth, and improving overall function.
7. Diagnostic Imaging & Precision Diagnostics (CBCT, EMG, Ultrasound)
Advanced diagnostic imaging provides an objective, data-driven evaluation of your temporomandibular joint's structure and function. Unlike treatments based solely on symptoms, this approach uses specialized technology to pinpoint the exact anatomical and physiological causes of your TMJ disorder. This precision allows for highly targeted and effective treatment planning, making it a cornerstone of modern TMJ care.
This process involves tools like Cone Beam Computed Tomography (CBCT) to visualize bone health, Electromyography (EMG) to measure muscle activity, and high-resolution ultrasound to assess soft tissues like the articular disc. By creating a complete picture of your jaw system, specialists can move beyond guesswork and design a personalized protocol that addresses the specific sources of your pain and dysfunction. This makes precision diagnostics one of the best TMJ treatments for complex cases.
Who Benefits from This Approach?
Precision diagnostics is invaluable for patients whose symptoms don't respond to initial conservative therapies or for those with complex presentations. For example, a CBCT scan might identify early degenerative changes like osteoarthritis, prompting the use of regenerative therapies before the condition worsens. Similarly, a patient with chronic muscle pain could use EMG biofeedback to see a measurable reduction in jaw clenching activity after just a few weeks of targeted therapy. Ultrasound can reveal the exact position and integrity of the TMJ disc, guiding whether a conservative or more invasive approach is necessary.
Practical Tips for Success
To get the most out of advanced diagnostics, it's important to use the data to guide every step of your treatment.
- Establish a Baseline: Obtain initial imaging, like a CBCT, to guide the first phase of treatment and serve as a benchmark for progress.
- Integrate Technology: Use tools like EMG biofeedback during myofunctional therapy sessions to provide real-time feedback and accelerate muscle retraining.
- Educate Yourself: Ask your specialist to review your imaging with you. Understanding the "why" behind your diagnosis can significantly improve your commitment to the treatment plan.
- Track Your Progress: Use follow-up imaging to objectively measure treatment outcomes, such as documenting cartilage health improvements after regenerative injections.
By leveraging advanced technologies to see precisely what is happening inside the jaw joint and surrounding muscles, diagnostic imaging allows for a truly personalized and evidence-based treatment strategy.
8. Pediatric Tongue-Tie Evaluation & Laser Frenectomy
Ankyloglossia, commonly known as tongue-tie, is a congenital condition where a restrictive band of tissue (the lingual frenulum) tethers the tongue's tip to the floor of the mouth. This restriction limits tongue mobility, which can disrupt feeding, swallowing, speech, and proper craniofacial development. Over time, the body creates harmful compensatory muscle patterns to overcome this limitation, directly contributing to future TMJ disorders, sleep-breathing issues, and orthodontic problems.
Laser frenectomy is a precise, minimally invasive procedure that uses concentrated light energy to release this restrictive tissue. Compared to traditional surgical methods, it offers minimal bleeding, reduced discomfort, and faster healing. Addressing a tongue-tie early, ideally in infancy, is a powerful preventative strategy, making it one of the best TMJ treatments by correcting the root cause before dysfunction and pain can develop.
Who Benefits from This Approach?
Early intervention is key, but individuals of all ages can benefit. An infant struggling with breastfeeding may achieve a proper latch and feeding efficiency soon after the procedure. A toddler with a speech delay often shows marked improvement in articulation when the tongue is freed. For adolescents and adults, a frenectomy, often combined with myofunctional therapy, can help resolve long-standing issues like sleep apnea, chronic headaches, and persistent jaw tension by finally allowing the tongue and facial muscles to function correctly.
Practical Tips for Success
A successful outcome depends on a collaborative and comprehensive approach.
- Seek Specialized Diagnosis: Ensure a definitive diagnosis is made by a trained pediatric dentist or provider experienced in identifying tethered oral tissues.
- Involve a Lactation Consultant: For infants, a pre-procedure evaluation by a lactation consultant is crucial to document feeding dysfunction and guide post-procedure care.
- Prioritize Post-Op Therapy: Schedule orofacial myofunctional therapy to begin 1-2 weeks after the procedure to retrain the tongue and establish correct functional patterns.
- Perform Stretching Exercises: Parents must be diligent with prescribed post-operative stretching exercises to prevent the frenulum from reattaching and to encourage new muscle memory.
By identifying and treating tongue-tie at the earliest opportunity, it’s possible to prevent the cascade of compensatory habits that lead to TMJ pain and airway compromise, promoting lifelong oral and systemic health.
8-Point Comparison of Top TMJ Treatments
| Treatment | Implementation Complexity 🔄 | Resource Requirements ⚡ | Expected Outcomes 📊 | Ideal Use Cases ⭐ | Key Advantages & Tips 💡 |
|---|---|---|---|---|---|
| Physical Therapy & Myofunctional Therapy | Moderate — specialist training + high patient compliance | Low equipment; time‑intensive (8–12 week programs, daily home exercises) | Gradual functional improvement; noticeable 6–12 weeks, significant 3–6 months | Postural/orofacial dysfunction, breathing/swallowing‑related TMJ issues; all ages | Non‑invasive, addresses root causes; maintain daily routine, combine with nasal breathing and follow‑ups |
| Prolotherapy (Proliferation Therapy) | Moderate — injection skills and protocolized sessions (4–6) | Clinic visits, often ultrasound guidance; brief downtime after injections | Progressive ligament strengthening; improvement 3–6 months, full effect 6–12 months | Ligamentous laxity, chronic instability, post‑injury TMJ cases | Targets structural instability; complete full series, expect short post‑injection inflammation |
| Platelet‑Rich Fibrin (PRF) Injections | Moderate — venipuncture, processing, injection technique (2–3 sessions) | Centrifuge equipment, trained staff, office procedure; usually out‑of‑pocket | Reduced inflammation, improved joint healing; partial 2–4 weeks, optimal 8–12 weeks after series | Early OA, intra/extra‑articular regenerative needs, post‑traumatic joints | Autologous regenerative approach; avoid NSAIDs pre/post, stay hydrated before blood draw |
| Cold Laser Therapy (LLLT) | Low — device operation training; short, repeatable sessions | Laser device, multiple weekly visits (10–15 min/session over 4–8 weeks) | Rapid pain reduction in acute flares; sustained benefit requires repeat sessions | Acute inflammatory flares, adjunct pain control, faster soft‑tissue healing | Non‑invasive and fast; best used as adjunct to biomechanical correction rather than sole therapy |
| Buteyko Breathing Technique | Moderate — certified instruction + consistent daily practice (8–12 weeks) | Minimal equipment; significant time/practice commitment | Improved nasal breathing and sleep quality; 6–12 weeks for clinical change | Mouth‑breathing, sleep‑breathing disorders, TMJ tension from airway dysfunction | Addresses airway root cause; combine with myofunctional therapy, use nasal hygiene, practice regularly |
| Oral Appliance Therapy (Custom Bite Splints & MADs) | Low–Moderate — dental fabrication and adjustment (2–4 week adaptation) | Lab fabrication, dental follow‑ups, occasional replacements every years | Often immediate symptom relief; optimal benefits after 4–6 weeks of consistent use | Bruxism, nighttime clenching, mild–moderate OSA, tooth protection | Immediate protection and sleep improvement; requires nightly compliance and periodic maintenance |
| Diagnostic Imaging & Precision Diagnostics (CBCT, EMG, Ultrasound) | High — specialized equipment and interpretation expertise | CBCT/EMG/ultrasound devices, trained operators, higher upfront cost | Objective identification of structural/physiologic pathology; guides targeted treatment and documents outcomes | Complex/refractory cases, pre‑surgical planning, when objective baseline is needed | Enables personalized, evidence‑based plans; obtain baseline imaging and use EMG biofeedback during therapy |
| Pediatric Tongue‑Tie Evaluation & Laser Frenectomy | Low–Moderate — assessment + brief laser procedure; requires post‑op therapy | CO₂ laser or equivalent, pediatric expertise, myofunctional follow‑up | Immediate feeding improvement; full functional establishment 4–12 weeks with therapy | Infants with feeding problems, speech/swallowing deficits, prevention of future TMJ/airway issues | Fast, low‑bleed release that prevents compensatory patterns; screen early and start post‑op myofunctional therapy |
Crafting Your Personalized Path to a Pain-Free Life
Navigating the complex landscape of temporomandibular joint disorder (TMD) can feel daunting, but this exploration of the best TMJ treatments should leave you feeling empowered, not overwhelmed. We've journeyed through a wide array of innovative and foundational therapies, from the muscle-retraining power of Orofacial Myofunctional Therapy and Buteyko Breathing to the joint-stabilizing potential of Prolotherapy and the regenerative capabilities of Platelet-Rich Fibrin (PRF). Each option represents a powerful tool in the fight against jaw pain, headaches, and dysfunction.
The single most important takeaway is that there is no universal "best" treatment, only the best TMJ treatment for you. Lasting relief rarely comes from a single, isolated intervention. Instead, it emerges from a thoughtfully constructed, personalized plan that addresses the root cause of your symptoms, rather than just masking the pain. True healing requires a shift in perspective: from simply treating a painful joint to restoring the harmony of the entire craniofacial and airway system.
Synthesizing Your Treatment Strategy
Think of the therapies we've discussed as building blocks for your recovery. An effective, sustainable plan often involves a multi-faceted approach, where different treatments work synergistically to produce a result greater than the sum of their parts.
Consider this practical scenario:
- Initial Phase (Diagnosis & Stabilization): Your journey might begin with advanced diagnostics like Cone Beam Computed Tomography (CBCT) to get a crystal-clear picture of your joint anatomy and airway. This could be followed by regenerative PRF injections to reduce inflammation and kickstart tissue repair within the joint capsule itself.
- Intermediate Phase (Functional Correction): With the acute pain managed, the focus shifts to correcting the underlying functional issues. Orofacial Myofunctional Therapy would be introduced to retrain your tongue posture and swallowing patterns, while Physical Therapy helps release chronic muscle tension in the neck and shoulders.
- Supportive & Long-Term Phase (Systemic Health): To support these changes, you might incorporate Cold Laser Therapy to accelerate healing and further reduce any lingering discomfort. If an airway issue is identified, a custom oral appliance could be fabricated to ensure proper jaw positioning and optimal breathing during sleep, preventing the clenching and grinding that contributed to the initial problem.
This integrated model ensures that you are not just putting a bandage on the symptoms but are actively rebuilding a healthier, more resilient system from the ground up.
The Power of an Interdisciplinary, Airway-Focused Approach
The common thread connecting the most successful outcomes in TMJ care is the recognition that the jaw does not function in isolation. Its health is inextricably linked to breathing, posture, sleep quality, and even pediatric development, as seen in the critical role of tongue-tie evaluations. This is why seeking a specialist who operates with an interdisciplinary, airway-focused philosophy is paramount.
A practitioner like Dr. Greg D. Larson at the Pain and Sleep Therapy Center looks beyond the temporomandibular joint. They ask deeper questions: Is compromised breathing during sleep causing nocturnal bruxism? Are dysfunctional muscle patterns from childhood still contributing to adult facial pain? By connecting these dots, they can assemble the right combination of regenerative, functional, and supportive therapies tailored to your unique anatomical and physiological needs.
Your path forward begins with a commitment to seeking this kind of comprehensive care. Stop chasing temporary fixes and start building a foundation for sustainable health and comfort. The journey to a pain-free life is not about finding a magic bullet; it's about meticulously crafting a personalized strategy that restores function, promotes healing, and empowers you to reclaim control over your well-being.
If you are ready to move beyond symptom management and address the root cause of your TMJ pain with a truly comprehensive, airway-focused plan, we invite you to take the next step. The team at the Pain and Sleep Therapy Center specializes in creating personalized treatment protocols that integrate the very best TMJ treatments discussed here. Schedule your consultation today to begin your journey toward lasting relief at the Pain and Sleep Therapy Center.





